Overview
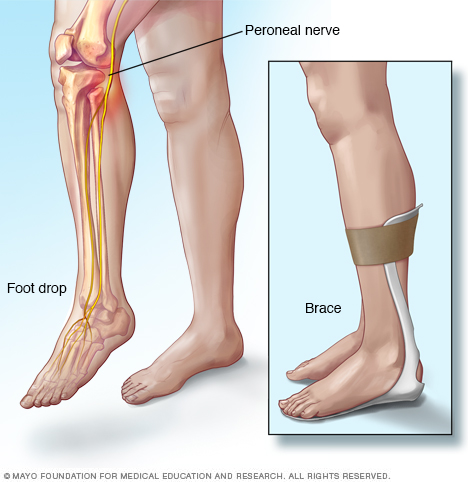
Foot drop, sometimes called drop foot, is a general term for difficulty lifting the front part of the foot. If you have foot drop, the front of your foot might drag on the ground when you walk.
Foot drop isn't a disease. Rather, it is a sign of an underlying neurological, muscular or anatomical problem.
Sometimes foot drop is temporary, but it can be permanent. If you have foot drop, you might need to wear a brace on your ankle and foot to support the foot and hold it in position.
Symptoms
Foot drop makes it difficult to lift the front part of the foot, so it might drag on the floor when you walk. To help the foot clear the floor, a person with foot drop may raise the thigh more than usual when walking, as though climbing stairs. This unusual kind of walking, called steppage gait, might cause the foot to slap down onto the floor with each step. In some cases, the skin on the top of the foot and toes feels numb.
Depending on the cause, foot drop can affect one or both feet.
When to see a doctor
If your toes drag on the floor when you walk, consult your doctor.
Causes
Foot drop is caused by weakness or paralysis of the muscles involved in lifting the front part of the foot. Causes of foot drop might include:
-
Nerve injury. The most common cause of foot drop is compression of a nerve in the leg that controls the muscles involved in lifting the foot. This nerve is called the peroneal nerve. A serious knee injury can lead to the nerve being compressed. It can also be injured during hip or knee replacement surgery, which may cause foot drop.
A nerve root injury — "pinched nerve" — in the spine also can cause foot drop. People who have diabetes are more susceptible to nerve disorders, which are associated with foot drop.
- Muscle or nerve disorders. Various forms of muscular dystrophy, an inherited disease that causes progressive muscle weakness, can contribute to foot drop. So can other neurologic disorders, such as polio or Charcot-Marie-Tooth disease.
- Brain and spinal cord disorders. Disorders that affect the spinal cord or brain — such as stroke, multiple sclerosis or amyotrophic lateral sclerosis (ALS) — may cause foot drop.
Risk factors
The peroneal nerve controls the muscles that lift the foot. This nerve runs near the surface of the skin on the side of the knee closest to the hand. Activities that compress this nerve can increase the risk of foot drop. Examples include:
- Leg crossing. People who habitually cross their legs can compress the peroneal nerve on their uppermost leg.
- Prolonged kneeling. Occupations that involve prolonged squatting or kneeling — such as picking strawberries or laying floor tile — can result in foot drop.
- Wearing a leg cast. Plaster casts that enclose the ankle and end just below the knee can exert pressure on the peroneal nerve.
Diagnosis
Foot drop is usually diagnosed during a physical exam. Your health care provider will watch you walk and check your leg muscles for weakness. Your provider also may check for numbness on your shin and on the top of your foot and toes.
Imaging tests
Foot drop is sometimes caused by a mass pushing on a nerve. This can be an overgrowth of bone in the spinal canal or a tumor or cyst pressing on the nerve in the knee or spine. Imaging tests can help pinpoint these types of problems.
- X-rays. Plain X-rays use a low level of radiation to visualize a soft tissue mass or a bone lesion that might be causing your symptoms.
- Ultrasound. This technology, which uses sound waves to create images of internal structures, can check for cysts or tumors on the nerve or show swelling on the nerve from compression.
- CT scan. This combines X-ray images taken from many different angles to form cross-sectional views of structures within the body.
- Magnetic resonance imaging (MRI). This test uses radio waves and a strong magnetic field to create detailed images of bones and soft tissues. MRI is particularly useful in visualizing soft tissue lesions that may be compressing a nerve.
Nerve tests
Electromyography (EMG) and nerve conduction studies measure electrical activity in the muscles and nerves. These tests can be uncomfortable, but they're useful in determining the location of the damage along the affected nerve.
Treatment
Treatment for foot drop depends on the cause. If the cause is successfully treated, foot drop might improve or even disappear. If the cause can't be treated, foot drop can be permanent.
Treatment for foot drop might include:
- Braces or splints. A brace on your ankle and foot or splint that fits into your shoe can help hold your foot in a normal position.
- Physical therapy. Exercises can strengthen your leg muscles and help you maintain the range of motion in your knee and ankle. These exercises might improve gait problems associated with foot drop. Stretching exercises are particularly important to prevent the stiffness in the calf and heel.
- Nerve stimulation. Sometimes stimulating the nerve that lifts the foot improves foot drop.
- Surgery. Depending upon the cause, and if your foot drop is relatively new, nerve surgery might be helpful. If foot drop is long-standing, your doctor might suggest surgery that transfers a working tendon to a different part of the foot to improve function.
Lifestyle and home remedies
Because foot drop can increase your risk of tripping and falling, consider taking these precautions around your house:
- Keep all floors clear of clutter.
- Avoid the use of throw rugs.
- Move electrical cords away from walkways.
- Make sure rooms and stairways are well-lit.
- Place fluorescent tape on the top and bottom steps of stairways.
Preparing for an appointment
You're likely to start by seeing your family care provider. Depending on the suspected cause of foot drop, you may be referred to a doctor who specializes in brain and nerve disorders, called a neurologist.
Here's some information to help you get ready for your appointment.
What you can do
Make a list of:
- Your symptoms, including ones that seem unrelated to the reason for which you scheduled the appointment, and when they began.
- Key personal information, including major stresses or recent life changes.
- All medications, vitamins or supplements you take, including doses.
- Questions to ask your care provider.
For foot drop, questions to ask your care provider include:
- What's causing my symptoms?
- What tests do I need?
- Is my condition likely temporary or chronic?
- What treatment do you recommend?
- Do you have brochures or other printed material I can have?
Don't hesitate to ask other questions.
What to expect from your doctor
Your care provider is likely to ask questions, such as:
- Are your symptoms present all the time, or do they come and go?
- Does anything seem to make your symptoms better?
- Does anything seem to make your symptoms worse?
- Do you notice weakness in your legs?
- Does your foot slap the floor when you walk?
- Do you have numbness or tingling in your foot or leg?
- Do you have pain? If so, what is it like and where is it located?
- Do you have a history of diabetes?
- Do you have other muscle weakness?
© 1998-2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use


