Overview
Inflammatory bowel disease (IBD) is a term that describes disorders involving long-standing (chronic) inflammation of tissues in your digestive tract. Types of IBD include:
- Ulcerative colitis. This condition involves inflammation and sores (ulcers) along the lining of your large intestine (colon) and rectum.
- Crohn's disease. This type of IBD is characterized by inflammation of the lining of your digestive tract, which often can involve the deeper layers of the digestive tract. Crohn's disease most commonly affects the small intestine. However, it can also affect the large intestine and uncommonly, the upper gastrointestinal tract.
Both ulcerative colitis and Crohn's disease usually are characterized by diarrhea, rectal bleeding, abdominal pain, fatigue and weight loss.
For some people, IBD is only a mild illness. For others, it's a debilitating condition that can lead to life-threatening complications.
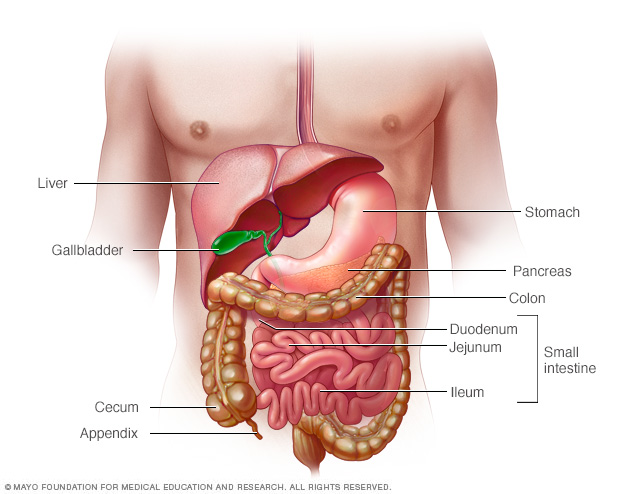
Symptoms
Inflammatory bowel disease symptoms vary, depending on the severity of inflammation and where it occurs. Symptoms may range from mild to severe. You are likely to have periods of active illness followed by periods of remission.
Signs and symptoms that are common to both Crohn's disease and ulcerative colitis include:
- Diarrhea
- Fatigue
- Abdominal pain and cramping
- Blood in your stool
- Reduced appetite
- Unintended weight loss
When to see a doctor
See your doctor if you experience a persistent change in your bowel habits or if you have any of the signs and symptoms of inflammatory bowel disease. Although inflammatory bowel disease usually isn't fatal, it's a serious disease that, in some cases, may cause life-threatening complications.
Causes
The exact cause of inflammatory bowel disease remains unknown. Previously, diet and stress were suspected, but now doctors know that these factors may aggravate but aren't the cause of IBD.
One possible cause is an immune system malfunction. When your immune system tries to fight off an invading virus or bacterium, an atypical immune response causes the immune system to attack the cells in the digestive tract, too.
Several gene mutations have been associated with IBD. Heredity also seems to play a role in that IBD is more common in people who have family members with the disease. However, most people with IBD don't have this family history.
Risk factors
- Age. Most people who develop IBD are diagnosed before they're 30 years old. But some people don't develop the disease until their 50s or 60s.
- Race or ethnicity. Although IBD is more common in white people, it can occur in any race. Cases are also increasing in other races and ethnicities.
- Family history. You're at higher risk if you have a close relative — such as a parent, sibling or child — with the disease.
-
Cigarette smoking. Cigarette smoking is the most important controllable risk factor for developing Crohn's disease.
Smoking may help prevent ulcerative colitis. However, its harm to overall health outweighs any benefit, and quitting smoking can improve the general health of your digestive tract, as well as provide many other health benefits.
- Nonsteroidal anti-inflammatory medications. These include ibuprofen (Advil, Motrin IB, others), naproxen sodium (Aleve), diclofenac sodium and others. These medications may increase the risk of developing IBD or worsen the disease in people who have IBD.
Complications
Ulcerative colitis and Crohn's disease have some complications in common and others that are specific to each condition. Complications found in both conditions may include:
- Colon cancer. Having ulcerative colitis or Crohn's disease that affects most of your colon can increase your risk of colon cancer. Screening for cancer with a colonoscopy at regular intervals begins usually about 8 to 10 years after the diagnosis is made. Ask your doctor when and how frequently you need to have this test done.
- Skin, eye and joint inflammation. Certain disorders, including arthritis, skin lesions and eye inflammation (uveitis), may occur during IBD flare-ups.
- Medication side effects. Certain medications for IBD are associated with a risk of infections. Some carry a small risk of developing certain cancers. Corticosteroids can be associated with a risk of osteoporosis, high blood pressure and other conditions.
- Primary sclerosing cholangitis. In this rather uncommon condition seen in people with IBD, inflammation causes scarring within the bile ducts. This scarring eventually narrows the ducts, restricting bile flow. This can eventually cause liver damage.
- Blood clots. IBD increases the risk of blood clots in veins and arteries.
- Severe dehydration. Excessive diarrhea can result in dehydration.
Complications of Crohn's disease may include:
- Bowel obstruction. Crohn's disease affects the full thickness of the intestinal wall. Over time, parts of the bowel can thicken and narrow, which may block the flow of digestive contents. You may require surgery to remove the diseased portion of your bowel.
- Malnutrition. Diarrhea, abdominal pain and cramping may make it difficult for you to eat or for your intestine to absorb enough nutrients to keep you nourished. It's also common to develop anemia due to low iron or vitamin B-12 caused by the disease.
- Fistulas. Sometimes inflammation can extend completely through the intestinal wall, creating a fistula — an atypical connection between different body parts. Fistulas near or around the anal area (perianal) are the most common kind. But they can also occur internally or toward the wall of the abdominal area. In some cases, a fistula may become infected and form an infected pocket of pus known as an abscess.
- Anal fissure. This is a small tear in the tissue that lines the anus or in the skin around the anus where infections can occur. It's often associated with painful bowel movements and may lead to a perianal fistula.
Complications of ulcerative colitis may include:
- Toxic megacolon. Ulcerative colitis may cause the colon to rapidly widen and swell, a serious condition known as toxic megacolon.
- A hole in the colon (perforated colon). A perforated colon most commonly is caused by toxic megacolon, but it may also occur on its own.
Diagnosis
To help confirm a diagnosis of IBD, you will need a combination of tests and procedures:
Lab tests
- Tests for anemia or infection. Your provider may suggest blood tests to check for anemia — a condition in which there aren't enough red blood cells to carry adequate oxygen to your tissues — or to check for signs of infection from bacteria or viruses.
- Stool studies. You may need to provide a stool sample so that your provider can test for hidden (occult) blood or organisms, such as parasites, in your stool.
Endoscopic procedures
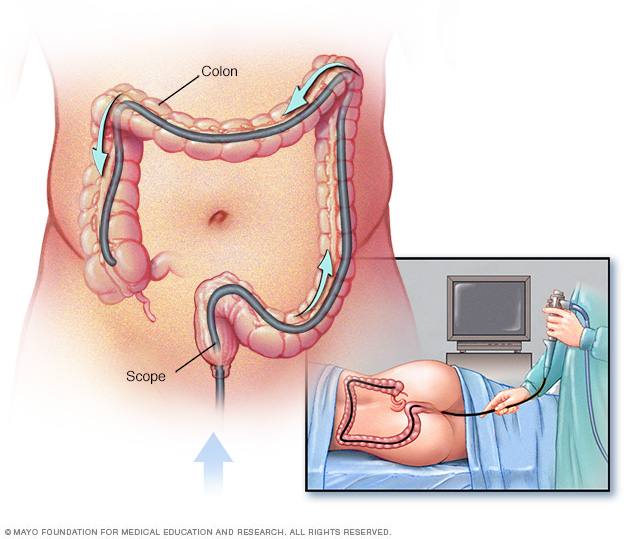
- Colonoscopy. This exam allows your provider to view your entire colon using a thin, flexible, lighted tube with a camera at the end. During the procedure, small samples of tissue (biopsy) may be taken for laboratory analysis. A biopsy is the way to make the diagnosis of IBD versus other forms of inflammation.
- Flexible sigmoidoscopy. Your provider uses a slender, flexible, lighted tube to examine the rectum and sigmoid, the last portion of your colon. If your colon is severely inflamed, your provider may perform this test instead of a full colonoscopy.
- Upper endoscopy. In this procedure, your provider uses a slender, flexible, lighted tube to examine the esophagus, stomach and first part of the small intestine (duodenum). While it is rare for these areas to be involved with Crohn's disease, this test may be recommended if you are having nausea and vomiting, difficulty eating, or upper abdominal pain.
- Capsule endoscopy. This test is sometimes used to help diagnose Crohn's disease involving your small intestine. You swallow a capsule that has a camera in it. The images are transmitted to a recorder you wear on your belt, after which the capsule exits your body painlessly in your stool. You may still need an endoscopy with a biopsy to confirm a diagnosis of Crohn's disease. Capsule endoscopy should not be performed if a bowel obstruction is suspected.
- Balloon-assisted enteroscopy. For this test, a scope is used in conjunction with a device called an overtube. This enables the technician to look further into the small bowel where standard endoscopes don't reach. This technique is useful when a capsule endoscopy shows abnormalities, but the diagnosis is still in question.
Imaging procedures
- X-ray. If you have severe symptoms, your provider may use a standard X-ray of your abdominal area to rule out serious complications, such as megacolon or a perforated colon.
- Computerized tomography (CT) scan. You may have a CT scan — a special X-ray technique that provides more detail than a standard X-ray does. This test looks at the entire bowel as well as at tissues outside the bowel. CT enterography is a special CT scan that provides better images of the small bowel. This test has replaced barium X-rays in most medical centers.
- Magnetic resonance imaging (MRI). An MRI scanner uses a magnetic field and radio waves to create detailed images of organs and tissues. An MRI is particularly useful for evaluating a fistula around the anal area (pelvic MRI) or the small intestine (MR enterography). Unlike CT, there is no radiation exposure with MRI.
Treatment
The goal of inflammatory bowel disease treatment is to reduce the inflammation that triggers your signs and symptoms. In the best cases, this may lead not only to symptom relief but also to long-term remission and reduced risks of complications. IBD treatment usually involves either drug therapy or surgery.
Anti-inflammatory drugs
Anti-inflammatory drugs are often the first step in the treatment of ulcerative colitis, typically for mild to moderate disease. Anti-inflammatories include aminosalicylates, such as mesalamine (Delzicol, Rowasa, others), balsalazide (Colazal) and olsalazine (Dipentum).
Time-limited courses of corticosteroids are also used to induce remission. In addition to being anti-inflammatory, steroids are immunosuppressing. Which medication you take depends on the area of your colon that's affected.
Immune system suppressors
These drugs work in a variety of ways to suppress the immune response that releases inflammation-inducing chemicals into the body. When released, these chemicals can damage the lining of the digestive tract.
Some examples of immunosuppressant drugs include azathioprine (Azasan, Imuran), mercaptopurine (Purinethol, Purixan) and methotrexate (Trexall).
More recently, orally delivered agents also known as "small molecules" have become available for IBD treatment. These include tofacitinib (Xeljanz), upadacitinib (Rinvoq) and ozanimod (Zeposia).
The U.S. Food and Drug Administration (FDA) recently issued a warning about tofacitinib, stating that preliminary studies show an increased risk of serious heart-related problems and cancer from taking this drug. If you're taking tofacitinib for ulcerative colitis, don't stop taking the medication without first talking with your doctor.
Biologics
Biologics are a newer category of therapy in which therapy is directed toward neutralizing proteins in the body that are causing inflammation. Some are administered via intravenous (IV) infusions and others are injections you give yourself. Examples include infliximab (Remicade), adalimumab (Humira), golimumab (Simponi), certolizumab (Cimzia), vedolizumab (Entyvio), ustekinumab (Stelara), and risankizumab (Skyrizi).
Antibiotics
Antibiotics may be used in addition to other medications or when infection is a concern — in cases of perianal Crohn's disease, for example. Frequently prescribed antibiotics include ciprofloxacin (Cipro) and metronidazole (Flagyl).
Other medications and supplements
In addition to controlling inflammation, some medications may help relieve your signs and symptoms, but always talk to your doctor before taking any over-the-counter medications. Depending on the severity of your IBD, your doctor may recommend one or more of the following:
-
Anti-diarrheal medications. A fiber supplement — such as psyllium powder (Metamucil) or methylcellulose (Citrucel) — can help relieve mild to moderate diarrhea by adding bulk to your stool. For more severe diarrhea, loperamide (Imodium A-D) may be effective.
These medications could be ineffective or detrimental in some people with strictures or certain infections. Please consult your doctor before taking these medications.
- Pain relievers. For mild pain, your doctor may recommend acetaminophen (Tylenol, others). However, ibuprofen (Advil, Motrin IB, others), naproxen sodium (Aleve) and diclofenac sodium likely will make your symptoms worse and can make your disease worse as well.
- Vitamins and supplements. If you're not absorbing enough nutrients, your doctor may recommend vitamins and nutritional supplements.
Nutritional support
When weight loss is severe, your doctor may recommend a special diet given via a feeding tube (enteral nutrition) or nutrients injected into a vein (parenteral nutrition) to treat your IBD. This can improve your overall nutrition and allow the bowel to rest. Bowel rest can reduce inflammation in the short term.
If you have a stenosis or stricture in the bowel, your doctor may recommend a low-residue diet. This will help to minimize the chance that undigested food will get stuck in the narrowed part of the bowel and lead to a blockage.
Surgery
If diet and lifestyle changes, drug therapy, or other treatments don't relieve your IBD signs and symptoms, your provider may recommend surgery.
-
Surgery for ulcerative colitis. Surgery involves removal of the entire colon and rectum and the production of an internal pouch attached to the anus that allows bowel movements without a bag.
In some cases a pouch is not possible. Instead, surgeons create a permanent opening in your abdomen (ileal stoma) through which stool is passed for collection in an attached bag.
-
Surgery for Crohn's disease. Up to two-thirds of people with Crohn's disease will require at least one surgery in their lifetime. However, surgery does not cure Crohn's disease.
During surgery, your surgeon removes a damaged portion of your digestive tract and then reconnects the healthy sections. Surgery may also be used to close fistulas and drain abscesses.
The benefits of surgery for Crohn's disease are usually temporary. The disease often recurs, frequently near the reconnected tissue. The best approach is to follow surgery with medication to minimize the risk of recurrence.
Lifestyle and home remedies
Sometimes you may feel helpless when facing inflammatory bowel disease. But changes in your diet and lifestyle may help control your symptoms and lengthen the time between flare-ups.
Diet
There's no firm evidence that what you eat actually causes inflammatory bowel disease. But certain foods and beverages can aggravate your signs and symptoms, especially during a flare-up.
It can be helpful to keep a food diary to keep track of what you're eating, as well as how you feel. If you discover that some foods are causing your symptoms to flare, you can try eliminating those foods.
Here are some general dietary suggestions that may help you manage your condition:
- Limit dairy products. Many people with inflammatory bowel disease find that problems such as diarrhea, abdominal pain and gas improve by limiting or eliminating dairy products. You may be lactose intolerant — that is, your body can't digest the milk sugar (lactose) in dairy foods. Using an enzyme product such as Lactaid may help as well.
- Eat small meals. You may find that you feel better eating five or six small meals a day rather than two or three larger ones.
- Drink plenty of liquids. Try to drink plenty of liquids daily. Water is best. Alcohol and beverages that contain caffeine stimulate your intestines and can make diarrhea worse, while carbonated drinks frequently produce gas.
- Consider multivitamins. Because Crohn's disease can interfere with your ability to absorb nutrients and because your diet may be limited, multivitamin and mineral supplements are often helpful. Check with your doctor before taking any vitamins or supplements.
- Talk to a dietitian. If you begin to lose weight or your diet has become very limited, talk to a registered dietitian.
Smoking
Smoking increases your risk of developing Crohn's disease, and once you have it, smoking can make it worse. People with Crohn's disease who smoke are more likely to have relapses and need medications and repeat surgeries.
Smoking may help prevent ulcerative colitis. However, its harm to overall health outweighs any benefit, and quitting smoking can improve the general health of your digestive tract, as well as provide many other health benefits.
Stress
The association of stress with Crohn's disease is controversial, but many people who have the disease report symptom flares during high-stress periods. If you have trouble managing stress, try one of these strategies:
- Exercise. Even mild exercise can help reduce stress, relieve depression and normalize bowel function. Talk to your doctor about an exercise plan that's right for you.
- Biofeedback. This stress-reduction technique may train you to reduce muscle tension and slow your heart rate with the help of a feedback machine. The goal is to help you enter a relaxed state so that you can cope more easily with stress.
- Regular relaxation and breathing exercises. One way to cope with stress is to regularly relax and use techniques such as deep, slow breathing to calm down.
Alternative medicine
Many people with digestive disorders have used some form of complementary and alternative medicine. However, there are few well-designed studies of the safety and effectiveness of complementary and alternative medicine.
Researchers suspect that adding more of the beneficial bacteria (probiotics) that are normally found in the digestive tract might help combat IBD. Although research is limited, there is some evidence that adding probiotics along with other medications may be helpful, but this has not been proved.
Coping and support
IBD doesn't just affect you physically — it takes an emotional toll as well. If signs and symptoms are severe, your life may revolve around a constant need to run to the toilet. Even if your symptoms are mild, it can be difficult to be out in public. All of these factors can alter your life and may lead to depression. Here are some things you can do:
- Be informed. One of the best ways to be more in control is to find out as much as possible about inflammatory bowel disease. Look for information from reputable sources such as the Crohn's and Colitis Foundation.
- Join a support group. Although support groups aren't for everyone, they can provide valuable information about your condition as well as emotional support. Group members frequently know about the latest medical treatments or integrative therapies. You may also find it reassuring to be among others with IBD.
- Talk to a therapist. Some people find it helpful to consult a mental health professional who's familiar with inflammatory bowel disease and the emotional difficulties it can cause.
Although living with IBD can be discouraging, research is ongoing, and the outlook is improving.
Preparing for an appointment
Symptoms of inflammatory bowel disease may first prompt a visit to your primary health care provider. However, you may then be referred to a doctor who specializes in treating digestive disorders (gastroenterologist).
Because appointments can be brief, and there's often a lot of information to discuss, it's a good idea to be well prepared. Here's some information to help you get ready and what to expect from your provider.
What you can do
- Be aware of any pre-appointment restrictions. At the time you make the appointment, be sure to ask if there's anything you need to do in advance, such as restrict your diet.
- Write down any symptoms you're experiencing, including any that may seem unrelated to the reason for which you made the appointment.
- Write down key personal information, including any major stresses or recent life changes.
- Make a list of all medications, including over-the-counter medications and any vitamins or supplements that you're taking.
- Take a family member or friend along. Sometimes it can be difficult to remember everything during an appointment. Someone who accompanies you may remember something that you missed or forgot.
- Write down questions to ask your provider.
Preparing a list of questions beforehand may help you make the most of your visit. List your questions from most important to least important in case time runs out. For inflammatory bowel disease, some basic questions to ask include:
- What's causing these symptoms?
- Are there other possible causes for my symptoms?
- What kinds of tests do I need? Do these tests require any special preparation?
- Is this condition temporary or long lasting?
- What treatments are available, and which do you recommend?
- Are there any medications that I should avoid?
- What types of side effects can I expect from treatment?
- What sort of follow-up care do I need? How often do I need a colonoscopy?
- Are there any alternatives to the primary approach that you're suggesting?
- I have other health conditions. How can I best manage them together?
- Do I need to follow any dietary restrictions?
- Is there a generic alternative to the medicine you're prescribing?
- Are there brochures or other printed material that I can take with me? What websites do you recommend?
- Is there a risk to me or my child if I become pregnant?
- Is there a risk of complications to my partner's pregnancy if I have IBD and father a child?
- What is the risk to my child of developing IBD if I have it?
- Are there support groups for people with IBD and their families?
What to expect from your doctor
Your provider is likely to ask you a number of questions. Being ready to answer them may reserve time to go over points you want to spend more time on. Your provider may ask:
- When did you first begin experiencing symptoms?
- Have your symptoms been continuous or intermittent?
- How severe are your symptoms?
- Do you have abdominal pain?
- Have you had diarrhea? How often?
- Do you awaken from sleep during the night because of diarrhea?
- Is anyone else in your home sick with diarrhea?
- Have you lost weight unintentionally?
- Have you ever had liver problems, hepatitis or jaundice?
- Have you had problems with your joints, eyes or skin — including rashes and sores — or had sores in your mouth?
- Do you have a family history of inflammatory bowel disease?
- Do your symptoms affect your ability to work or do other activities?
- Does anything seem to improve your symptoms?
- Is there anything that you've noticed that makes your symptoms worse?
- Do you smoke?
- Do you take nonsteroidal anti-inflammatory drugs (NSAIDs), for example, ibuprofen (Advil, Motrin IB, others), naproxen sodium (Aleve) or diclofenac sodium (Voltaren)?
- Have you taken antibiotics recently?
- Have you recently traveled? If so, where?
© 1998-2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use


