Overview
Pulmonary atresia (uh-TREE-zhuh) is a heart problem present at birth. That means it is a congenital heart defect. In this condition, the valve that helps move blood from the heart to the lungs doesn't form correctly. The valve is called the pulmonary valve.
Instead of a valve that opens and closes, a solid sheet of tissue forms. So, blood can't travel its usual path to get oxygen from the lungs. Instead, some blood travels to the lungs through other natural passages within the heart and its arteries.
A baby in the womb needs these other passages. But they usually close soon after birth.
Pulmonary atresia is a life-threatening condition that needs emergency treatment. Treatment includes surgery to repair the heart and medicines to help the heart work better.
Symptoms
Symptoms of pulmonary atresia may be seen soon after birth. They can include:
- Blue or gray skin, lips or fingernails due to low oxygen levels. Depending on the skin color, these changes may be harder or easier to see.
- Fast breathing or shortness of breath.
- Tiring easily.
- Not feeding well.
When to see a doctor
Pulmonary atresia is most often found soon after birth. If your baby has symptoms of pulmonary atresia after you've left the hospital, get medical help right away.
Causes
The cause of pulmonary atresia is not clear. During the first six weeks of pregnancy, the baby's heart begins to form and starts beating. The major blood vessels that run to and from the heart also begin to develop during this critical time. It's at this point in a baby's development that a congenital heart defect such as pulmonary atresia may begin to develop.
To understand how pulmonary atresia occurs, it may be helpful to know how the heart works.
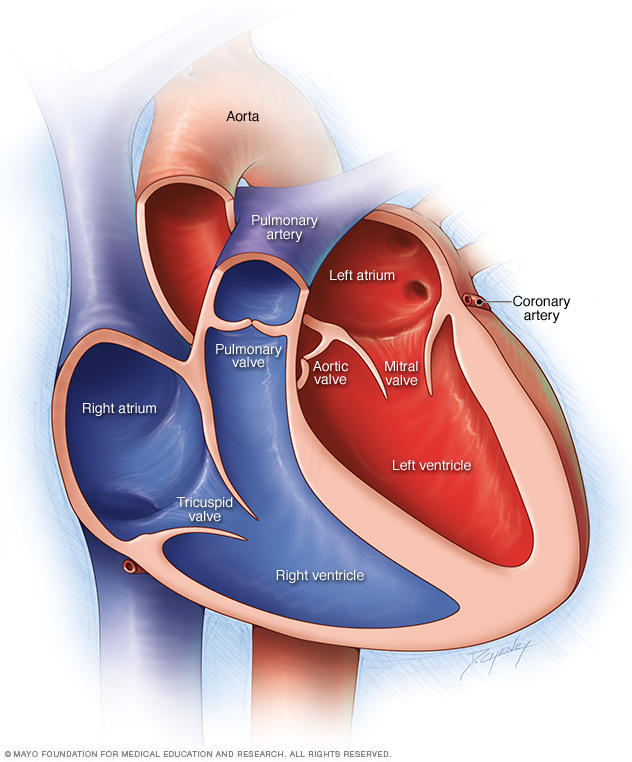
How the heart works
The typical heart is made of four chambers. There are two upper chambers, called atria, and two lower chambers, called ventricles.
The right side of the heart moves blood to the lungs. In the lungs, blood picks up oxygen and then returns it to the heart's left side. The left side of the heart then pumps the blood through the body's main artery, called the aorta. The blood goes to the rest of the body.
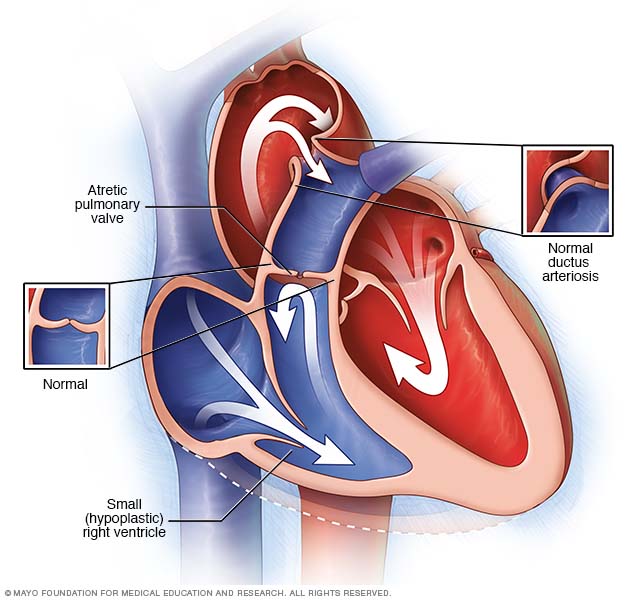
In pulmonary atresia, the pulmonary valve doesn't form as usual so it can't open. Blood can't flow from the right ventricle to the lungs.
Before birth, not having a pulmonary valve opening doesn't affect the baby's oxygen. That's because the baby gets oxygen from the tissue that connects the baby to the womb, called the placenta. The oxygen-rich blood from the placenta goes to the baby's right upper heart chamber.
The blood going into the right side of the baby's heart then passes through a hole between the top chambers of the baby's heart. The hole is called the foramen ovale. It lets oxygen-rich blood move to the rest of the baby's body through the aorta.
After birth, the lungs are needed for oxygen. In pulmonary atresia, without a working pulmonary valve, blood must find another way to reach the baby's lungs.
Blood from the right side of the heart can cross over the foramen ovale to the left heart. From there it can be pumped to the aorta. Newborn babies have a temporary opening called the ductus arteriosus between the aorta and the pulmonary artery. This opening lets some blood travel to the lungs. There the blood picks up oxygen to send to the rest of the baby's body.
The ductus arteriosus most often closes soon after birth. But medicines can keep it open.
Sometimes there's a second hole in the tissue between the main pumping chambers of the baby's heart. This hole is a ventricular septal defect (VSD).
The VSD lets blood flow from the right lower heart chamber to the left lower heart chamber. People with pulmonary atresia and a VSD often have other changes with the lungs and the arteries that bring blood to the lungs.
If there's no VSD, the right lower heart chamber gets little blood flow before birth. The chamber often doesn't form fully. This is a condition called pulmonary atresia with intact ventricular septum (PA/IVS).
Risk factors
Pulmonary atresia happens as the baby's heart is forming during pregnancy. Certain health conditions or illicit drug use during pregnancy may increase a baby's risk of pulmonary atresia or other congenital heart defects. Risk factors include:
- Obesity.
- Alcohol or tobacco use.
- Diabetes.
- Use of some types of medicines during pregnancy, such as certain acne and blood pressure medicines.
Some types of congenital heart defects occur in families. This means they are inherited. If you or someone in your family was born with a heart problem, including pulmonary atresia, ask your care team is genetic screening is right for you. Screening can help show the risk of certain congenital heart defects in future children.
Complications
Without treatment, pulmonary atresia most often leads to death. After surgery for pulmonary atresia, babies need regular health checkups throughout their lives to watch for complications.
Complications of pulmonary atresia may include:
- Bacterial infection of the inner lining of the heart and valves, called infectious endocarditis.
- Irregular heartbeats, called arrhythmias.
- Weakening of heart function.
Prevention
It might not be possible to prevent pulmonary atresia. But getting good prenatal care is important. Some things you can do before or during pregnancy might help lower your baby's risk of congenital heart defects. They include:
- Control other health conditions. If you have diabetes, keep your blood sugar in check. For other conditions that need medicines, talk to your healthcare professional about taking these medicines while pregnant.
- Don't smoke and don't be around others who smoke. If you smoke, quit. Smoking during pregnancy increases the risk of a congenital heart defect in the baby.
- Aim for a healthy weight. Obesity increases the risk of having a baby with a congenital heart defect.
- Get recommended vaccinations. Having rubella, also called German measles, during pregnancy can cause problems in a baby's heart development. A blood test done before pregnancy can determine if you're immune to rubella. A vaccine is available for those who aren't immune.
Diagnosis
Pulmonary atresia is usually diagnosed soon after birth. Tests are done to check the baby's heart health.
Tests
Tests to diagnose pulmonary atresia may include:
- Pulse oximetry. A sensor placed on the fingertip records the amount of oxygen in the blood. Too little oxygen may be a sign of a heart or lung problem.
- Chest X-ray. A chest X-ray shows the size and shape of the heart and lungs.
- Electrocardiogram (ECG or EKG). This quick and painless test records the electrical activity of the heart. It shows how the heart is beating. Sticky patches called electrodes are put on the chest and sometimes the arms and legs. Wires connect the patches to a computer, which prints or displays the results.
- Echocardiogram. This test uses sound waves to create pictures of the beating heart. An echocardiogram is usually the main test to diagnose pulmonary atresia. It shows how blood moves through the heart and heart valves. If an echocardiogram is done on a baby before birth, it's called a fetal echocardiogram.
- Cardiac catheterization. A doctor threads a thin tube called a catheter through a blood vessel in the arm or groin to an artery in the heart. Dye is sent through the catheter. This makes the heart arteries show up more clearly on an X-ray. The test can provide detailed information on blood flow and how the heart works. Certain heart treatments can be done during cardiac catheterization.
Treatment
Babies need emergency medical care for pulmonary atresia symptoms. The choice of surgeries or procedures depends on how severe the condition is.
Medications
Medicine may be given through an IV to keep the ductus arteriosus open. This is not a long-term treatment for pulmonary atresia. But it gives healthcare professionals more time to decide what type of surgery or procedure might be best.
Surgery or other procedures
Sometimes, pulmonary atresia treatment can be done using a long, thin tube called a catheter. A doctor places the tube into a large blood vessel in a baby's groin and guides it to the heart. Catheter-based procedures for pulmonary atresia include:
- Balloon atrial septostomy. A balloon is used to enlarge the natural hole in the wall between the upper chambers of the heart. This hole, called the foramen ovale, most often closes soon after birth. Making the hole larger lets blood move easily from the right side of the heart to the left side.
- Stent placement. A doctor may put a rigid tube called a stent in the ductus arteriosus to prevent it from closing. This keeps blood flowing to the lungs.
Babies with pulmonary atresia often need many heart surgeries over time. The type of heart surgery depends on the size of the child's lower right heart chamber and pulmonary artery.
Types of surgery for pulmonary atresia include:
- Shunting. This involves making a new route for blood to flow, called a bypass shunt. The shunt goes from the main blood vessel leading out of the heart, called the aorta, to the pulmonary arteries. This lets enough blood flow to the lungs. But most babies outgrow this shunt within a few months.
- Glenn procedure. In this surgery, one of the large veins that returns blood to the heart is joined to the pulmonary artery. Another large vein keeps blood flowing to the right side of the heart. The heart then pumps it through the pulmonary valve that's been repaired. This can help the right ventricle grow.
- Fontan procedure. If the right lower heart chamber stays too small to do its work, surgeons may use this procedure to make a pathway. The pathway lets most, if not all, of the blood coming to the heart to flow into the pulmonary artery.
- Heart transplant. In some cases, the heart is too damaged to fix. Then a heart transplant may be needed.
If the baby also has a ventricular septal defect (VSD), surgery is done to patch the hole. Then the surgeon makes a connection from the right pumping chamber to the pulmonary artery. This repair may use an artificial valve.
Lifestyle and home remedies
Here are some tips for caring for someone with pulmonary atresia after coming home from the hospital:
- Go to scheduled health checkups. A person born with pulmonary atresia needs regular checkups, even as an adult. A doctor trained in congenital heart diseases, called a congenital cardiologist, often provides care. Get recommended vaccines, including yearly flu vaccines.
- Ask about exercise and activity. Some children with a congenital heart defect may need to limit exercise or sports activities. However, many others with a congenital heart defect can participate in such activities. Your child's care team can tell you which sports and types of exercise are safe for your child.
- Practice good oral hygiene. Brushing and flossing teeth and getting regular dental checkups can help prevent infection.
- Ask about preventive antibiotics. Sometimes, a congenital heart defect can increase the risk of infection in the lining of the heart or heart valves. This infection is called infective endocarditis. Antibiotics may be recommended before dental procedures to prevent infection, especially for people who have a mechanical heart valve.
Coping and support
Talking with other parents who have a child with a congenital heart defect might give you comfort and support. Ask a member of your child's care team about local support groups.
Preparing for an appointment
Your baby is likely to be diagnosed with pulmonary atresia soon after birth while still in the hospital. Then you'll be referred to a doctor trained in heart diseases, called a cardiologist, for ongoing care.
Here's some information to help you get ready for your appointment.
What you can do
When you make the appointment, ask if there's anything you need to do before you go. For instance, you might need to fill out forms or restrict your child's diet. For some imaging tests, your child may need to not eat or drink for a time before the tests.
Take a family member or friend to the appointment, if possible. This person can help you remember the details you're given.
Make a list of:
- Your child's symptoms, including ones that don't seem linked to pulmonary atresia. Try to recall when you noticed them.
- Key personal facts, including family history of congenital heart defects, pulmonary hypertension, or other heart or lung diseases.
- All medicines, vitamins, or supplements that your child takes and the doses. Also list medicines you took while pregnant.
- Questions to ask your child's healthcare professional.
For pulmonary atresia, some questions to ask include:
- What are other possible causes for my child's symptoms or condition?
- What tests will my child need?
- What's the best treatment?
- What other treatments are there?
- Are there activities my child should not do?
- How often should my child be screened for changes?
- Can you suggest a specialist who treats congenital heart defects?
- Are there brochures or other printed material that I can have? What websites do you suggest?
Be sure to ask all the questions you have about your child's condition.
What to expect from your child's doctor
Be ready to answer questions, such as:
- Has anyone else in your family been diagnosed with pulmonary atresia or another congenital heart defect?
- Does your child always have symptoms or do the symptoms come and go?
- How bad are the symptoms?
- What, if anything, seems to make the symptoms better?
- What, if anything, seems to make the symptoms worse?
© 1998-2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use


