Overview
Pulmonary fibrosis is a lung disease that occurs when lung tissue becomes damaged and scarred. This thickened, stiff tissue makes it harder for the lungs to work properly. Pulmonary fibrosis worsens over time. Some people can stay stable for a long time, but the condition gets worse faster in others. As it gets worse, people become more and more short of breath.
The scarring that happens in pulmonary fibrosis can be caused by many things. Often, doctors and other healthcare professionals cannot pinpoint what's causing the problem. When a cause cannot be found, the condition is called idiopathic pulmonary fibrosis.
Idiopathic pulmonary fibrosis usually occurs in middle-aged and older adults. Sometimes pulmonary fibrosis is diagnosed in children and infants, but this is not common.
The lung damage caused by pulmonary fibrosis cannot be repaired. Medicines and therapies can sometimes help slow down the rate of fibrosis, ease symptoms and improve quality of life. For some people, a lung transplant might be an option.
Symptoms
Symptoms of pulmonary fibrosis may include:
- Shortness of breath.
- Dry cough.
- Extreme tiredness.
- Weight loss that's not intended.
- Aching muscles and joints.
- Widening and rounding of the tips of the fingers or toes, called clubbing.
How fast pulmonary fibrosis worsens over time and how severe the symptoms are can vary greatly from person to person. Some people become ill very quickly with severe disease. Others have moderate symptoms that worsen more slowly, over months or years.
When symptoms suddenly get worse
In people with pulmonary fibrosis, especially idiopathic pulmonary fibrosis, shortness of breath can suddenly get worse over a few weeks or days. This is called an acute exacerbation. It can be life-threatening. The cause of an acute exacerbation may be another condition or an illness, such as a lung infection. But usually the cause is not known.
When to see a doctor
If you have symptoms of pulmonary fibrosis, contact your doctor or other healthcare professional as soon as possible. If your symptoms get worse, especially if they get worse fast, contact your healthcare team right away.
Causes
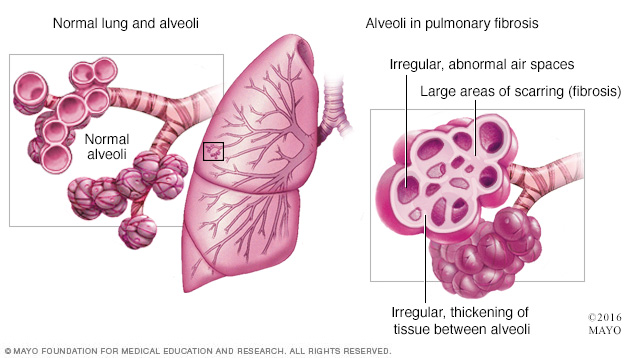
Pulmonary fibrosis is scarring and thickening of the tissue around and between the air sacs called alveoli in the lungs. These changes make it harder for oxygen to pass into the bloodstream.
Damage to the lungs that results in pulmonary fibrosis may be caused by many different things. Examples include long-term exposure to certain toxins, radiation therapy, some medicines and certain medical conditions. In some cases, the cause of pulmonary fibrosis is not known.
Your work and surroundings
The type of work you do and where you work or live could be the cause or part of the cause for pulmonary fibrosis. Having continuous or repeated contact with toxins or pollutants — substances that harm the quality of water, air or land — can damage your lungs, especially if you do not wear protective gear. Examples include:
- Silica dust.
- Asbestos fibers.
- Hard metal dusts.
- Wood, coal and grain dusts.
- Mold.
- Bird and animal droppings.
Radiation treatments
Some people who receive radiation therapy to the chest, such as for lung or breast cancer, show signs of lung damage months or sometimes years after treatment. How severe the damage is may depend on:
- How much of the lung was exposed to radiation.
- The total amount of radiation given.
- Whether chemotherapy also was used.
- Whether there is underlying lung disease.
Medicines
Many medicines can damage the lungs. Some examples include:
- Chemotherapy. Medicines designed to kill cancer cells, such as methotrexate (Trexall, Otrexup, others), bleomycin and cyclophosphamide (Cytoxan), can damage lung tissue.
- Heart medicines. Some medicines used to treat irregular heartbeats, such as amiodarone (Nexterone, Pacerone), may harm lung tissue.
- Some antibiotics. Antibiotics such as nitrofurantoin (Macrobid, Macrodantin) or ethambutol (Myambutol) can cause lung damage.
- Anti-inflammatory medicines. Certain anti-inflammatory medicines such as rituximab (Rituxan) or sulfasalazine (Azulfidine) can cause lung damage.
Medical conditions
Lung damage can also result from a number of conditions, including:
- Dermatomyositis, an inflammatory disease marked by muscle weakness and a skin rash.
- Lupus, a disease that occurs when the body's immune system attacks its own tissues and organs.
- Mixed connective tissue disease, which has a mix of symptoms of different disorders, such as lupus, scleroderma and polymyositis.
- Pneumonia, an infection that inflames the air sacs in one or both lungs.
- Polymyositis, an inflammatory disease that causes muscle weakness on both sides of the body.
- Rheumatoid arthritis, an inflammatory disease that affects joints and other body systems.
- Sarcoidosis, an inflammatory disease that most often affects the lungs and lymph nodes.
- Scleroderma, a group of rare diseases that involve hardening and tightening of the skin as well as problems inside the body.
Idiopathic pulmonary fibrosis
Many substances and conditions can lead to pulmonary fibrosis. Even so, in many people, the cause is never found. But risk factors such as smoking or exposure to air pollution could be related to the condition, even if the cause cannot be confirmed. Pulmonary fibrosis with no known cause is called idiopathic pulmonary fibrosis.
Many people with idiopathic pulmonary fibrosis also may have gastroesophageal reflux disease, also called GERD. This condition occurs when acid from the stomach flows back into the esophagus. GERD may be a risk factor for idiopathic pulmonary fibrosis or cause the condition to worsen faster. But more studies are needed.
Risk factors
Pulmonary fibrosis has been found in children and infants, but this is not common. Idiopathic pulmonary fibrosis is much more likely to affect middle-aged and older adults. Other types of pulmonary fibrosis, such as that caused by connective tissue disease, can occur in younger people.
Factors that can raise your risk of pulmonary fibrosis include:
- Smoking. If you smoke now or used to smoke, you're at a higher risk of pulmonary fibrosis than people who never smoked. People with emphysema are at higher risk, too.
- Certain types of work. You have a higher risk of developing pulmonary fibrosis if you work in mining, farming or construction. The risk also is higher if you have continuous or repeated contact with pollutants known to damage the lungs.
- Cancer treatments. Having radiation treatments to your chest or using certain chemotherapy medicines can raise your risk of pulmonary fibrosis.
- Genetics. Some types of pulmonary fibrosis run in families, so genes may play a role.
Complications
Complications of pulmonary fibrosis may include:
- High blood pressure in the lungs. Called pulmonary hypertension, this type of high blood pressure affects the arteries in the lungs. These are the pulmonary arteries. Stiff and thick arteries may slow down or block blood flow through the lungs. This raises the pressure inside the pulmonary arteries and the lower right heart chamber, called the right ventricle.
- Right-sided heart failure. This serious condition occurs when your heart's right chamber has to pump harder than usual to move blood through partly blocked pulmonary arteries.
- Respiratory failure. This is often the last stage of long-term lung disease. It occurs when blood oxygen levels fall dangerously low.
- Lung cancer. Long-standing pulmonary fibrosis increases your risk of developing lung cancer.
- Other lung problems. As pulmonary fibrosis gets worse over time, it may lead to serious problems such as blood clots in the lungs, a collapsed lung or lung infections.
Diagnosis
To diagnose pulmonary fibrosis, your doctor or other healthcare professional reviews your medical and family history and does a physical exam. You can talk about your symptoms and review any medicines you take. You also will likely be asked about any continuous or repeated contact with dusts, gases, chemicals or similar substances, especially through work.
During the physical exam, your healthcare professional listens carefully to your lungs while you breathe. Pulmonary fibrosis often occurs along with a crackling sound at the base of the lungs.
You may have one or more of these tests.
Imaging tests
- Chest X-ray. Images of the chest may show the scar tissue that is usually part of pulmonary fibrosis. Sometimes the chest X-ray may not show any changes. More tests may be needed to find out why you are short of breath.
- Computerized tomography (CT) scan. A CT scan combines X-ray images taken from many different angles to create images of structures inside the body. A high-resolution CT scan can be helpful in diagnosing pulmonary fibrosis and in finding out how much lung damage has occurred. Some kinds of fibrosis have certain patterns.
- Echocardiogram. An echocardiogram uses sound waves to look at the heart. The test can create pictures of the heart's structures. It also can create videos that show how the heart is working. This test can tell the amount of pressure in the arteries of the lungs and in the right side of the heart.
Lung function tests
Also called pulmonary function tests, these are done to find out how well your lungs are working:
- Spirometry. In this test, you breathe out quickly and forcefully through a tube connected to a machine. The machine measures how much air the lungs can hold and how quickly air moves in and out of the lungs.
- Lung volume test. This test measures the amount of air the lungs hold at different times when breathing in and out.
- Lung diffusion test. This test shows how well the body moves oxygen and carbon dioxide between the lungs and the blood.
- Pulse oximetry. This simple test uses a small device placed on one of the fingers to measure how much oxygen is in the blood. The percentage of oxygen in the blood is called oxygen saturation. Your healthcare professional may recommend a six-minute walking test with a check of your oxygen saturation.
- Exercise stress test. An exercise test on a treadmill or stationary bike may be used to monitor heart and lung function during activity.
- Arterial blood gas test. In this test, a sample of blood, usually taken from an artery in the wrist, is tested. The oxygen and carbon dioxide levels in the sample are measured.
In addition to showing whether you have pulmonary fibrosis, imaging and lung function tests can be used to check your condition over time and see how treatments are working.
Tissue sample
If other tests cannot find the cause of your condition, a small amount of lung tissue may need to be removed. This is called a biopsy. The biopsy sample is then examined in a laboratory to diagnose pulmonary fibrosis or rule out other conditions. One of these methods can be used to get a tissue sample:
Surgical biopsy. Although a surgical biopsy is invasive and has potential complications, it may be the only way to make the right diagnosis. This procedure may be done as a minimally invasive surgery called video-assisted thoracoscopic surgery (VATS). The biopsy also may be done as an open surgery called a thoracotomy.
During VATS, a surgeon inserts surgical instruments and a small camera through two or three small cuts between the ribs. The surgeon looks at the lungs on a video monitor while removing tissue samples from the lungs. During the surgery, a combination of medicines put you in a sleep-like state called general anesthesia.
During a thoracotomy, a surgeon removes a lung tissue sample through a cut that opens the chest between the ribs. This open surgery also is done using general anesthesia.
Bronchoscopy. In this procedure, very small tissue samples are removed — usually no larger than the head of a pin. A small, flexible tube called a bronchoscope is passed through the mouth or nose into the lungs to remove the samples. The tissue samples are sometimes too small to make the right diagnosis. But this form of biopsy also may be used to rule out other conditions.
Blood tests
You may have blood tests to look at your liver and kidney function. Blood tests also can check for and rule out other conditions.
Treatment
The lung scarring and thickening that occurs in pulmonary fibrosis cannot be repaired. And no current treatment has proved effective in stopping the disease from getting worse over time. Some treatments may improve symptoms for a time or slow how fast the disease worsens. Others may help improve quality of life.
Treatment depends on the cause of your pulmonary fibrosis. Doctors and other healthcare professionals evaluate how severe your condition is. Then together you can decide on the best treatment plan.
Medicines
If you have idiopathic pulmonary fibrosis, your healthcare professional may recommend the medicine pirfenidone (Esbriet) or nintedanib (Ofev). Both are approved by the U.S. Food and Drug Administration (FDA) for idiopathic pulmonary fibrosis. Nintedanib also is approved for other types of pulmonary fibrosis that get worse quickly. These medicines may help slow the worsening of pulmonary fibrosis and may prevent bouts when symptoms suddenly get worse.
Nintedanib can cause side effects such as diarrhea and nausea. Side effects of pirfenidone include nausea, loss of appetite and skin rash from sunlight. With either medicine, your healthcare professional uses regular blood tests to check how well the liver is working.
New medicines and therapies are being developed or tested in clinical trials but are not yet approved by the Food and Drug Administration (FDA). Researchers continue to study medicines to treat pulmonary fibrosis.
Doctors may recommend anti-acid medicines if you have symptoms of gastroesophageal reflux disease (GERD). GERD is a digestive condition that commonly occurs in people with idiopathic pulmonary fibrosis.
Oxygen therapy
Using extra oxygen, called supplemental oxygen, cannot stop lung damage, but it can:
- Make breathing and exercise easier.
- Prevent or lessen complications from low blood oxygen levels.
- Possibly lessen strain on the right side of the heart.
- Improve sleep and sense of well-being.
You may use oxygen when you sleep or exercise. But some people need oxygen all the time. Carrying a small tank of oxygen or using a portable oxygen concentrator can help you be more mobile.
Pulmonary rehabilitation
Pulmonary rehabilitation can help manage your symptoms and improve your ability to do daily tasks. Pulmonary rehabilitation programs focus on:
- Physical exercise to improve how much you can do.
- Breathing techniques that may improve how well your lungs use oxygen.
- Nutritional counseling.
- Emotional counseling and support.
- Education about your condition.
Symptoms
When symptoms suddenly get worse
When symptoms suddenly get worse, called an acute exacerbation, you may need more supplemental oxygen. In some cases, you may need mechanical ventilation in the hospital. In this treatment, a tube is guided into the lungs and attached to a machine that helps with breathing. Your healthcare professional may recommend antibiotics, corticosteroid medicines or other medicines when symptoms suddenly get worse.
Treatment
Lung transplant
A lung transplant may be an option for some people with pulmonary fibrosis. Having a lung transplant can improve your quality of life and allow you to live a longer life. But a lung transplant can involve complications such as rejection and infection. After a lung transplant, you take medicines for the rest of your life. You and your healthcare team may discuss a lung transplant if it's thought to be the right treatment option for your condition.
Lifestyle and home remedies
Being actively involved in your treatment and staying as healthy as possible are essential to living with pulmonary fibrosis. It's important to:
- Stop smoking. If you have lung disease, it is important to stop smoking. Talk with your healthcare team about options for quitting, including smoking cessation programs. These use proven techniques to help people quit. Because secondhand smoke can be harmful to your lungs, avoid being around people who are smoking.
- Avoid other things that can irritate your lungs. Breathing indoor pollutants, such as fumes from heating fuel or chemicals, can irritate your lungs. So can outdoor pollutants, such as dust or car exhaust.
- Eat well. People with lung disease may lose weight both because eating is not comfortable and because of the extra energy it takes to breathe. A healthy diet that contains enough calories is needed. Try to eat smaller meals more often during the day. A dietitian can give you more information on healthy eating for your condition.
- Get moving. Regular exercise can help you keep your lung function and manage your stress. Aim to include physical activity, such as walking or biking, into your daily routine. Talk to your healthcare team about what activities may be best for you. If over time you need help getting around, such as using a wheelchair, look for active movements you can do that do not require walking. One example is tai chi.
- Take time to rest. Make sure to get enough rest. Taking time to rest can help you have more energy and cope with the stress of your condition. If you have problems sleeping, talk with your healthcare team.
- Get vaccinated. Respiratory infections, such as colds and flu, can worsen symptoms of pulmonary fibrosis. Make sure that you get the pneumonia vaccine, an annual flu shot and COVID-19 vaccines. It's important that your family members also be vaccinated. Try to stay out of crowds when possible.
- Follow your treatment plan. You usually need ongoing treatment from your healthcare team. Follow the care team's instructions. Take your medicines as prescribed. Adjust your diet and exercise as needed. Attend pulmonary rehabilitation sessions. Go to all of your appointments and contact your care team if symptoms worsen.
Coping and support
Pulmonary fibrosis is a life-long lung condition that worsens over time. Having pulmonary fibrosis can cause fear, depression and stress. Here are some tips that may help you cope.
- Learn about your condition. Understanding the condition and treatments can help you and your family cope.
- Spend time with family and friends. Let them know how they can support and help you.
- Talk to your doctor or other healthcare professional. Talk about your condition and how you feel. If you're depressed or anxious, your doctor may suggest that you see a mental health professional.
- Join a support group. Meeting with other people who have pulmonary fibrosis may help. You can talk to people who have had similar symptoms or treatments. You also can learn ways to cope.
- Learn about palliative care services. As your condition gets worse, your care team may suggest palliative care services. These services provide support for severe symptoms, such as providing relief from pain and helping to improve other symptoms. They also help you and your family discuss end-of-life issues and plan advance directives.
Preparing for an appointment
If your primary care doctor or other healthcare professional suspects a serious lung problem, you are likely to be referred to a pulmonologist. This is a doctor with training and skills in diagnosing and treating lung disorders.
Pulmonary fibrosis is a serious and complex disease. Take a friend or family member with you to your appointment. That person can take notes while you talk with your healthcare team, provide emotional support and help remember information that you may forget or miss.
What you can do
To get ready for your appointment, make a list of:
- Any symptoms you're having and for how long.
- Key medical information, including recent hospital stays and any medical conditions.
- Key personal information, including any type of work that increases your risk or any recent travel.
- All medicines, vitamins, herbs and other supplements that you take, including the doses.
- Questions to ask the healthcare professional.
Some basic questions to ask include:
- What is likely causing my symptoms?
- What kinds of tests do I need?
- What treatments do you recommend?
- I have other health conditions. How will pulmonary fibrosis affect them?
- Are there any things that I should do or not do?
Feel free to ask other questions during your appointment.
© 1998-2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use


