Overview
Raynaud's (ray-NOSE) disease causes some areas of the body — such as fingers and toes — to feel numb and cold in response to cold temperatures or stress. In Raynaud's disease, smaller arteries that supply blood to the skin narrow. This limits blood flow to affected areas, which is called vasospasm.
Other names for this condition are:
- Raynaud's phenomenon.
- Raynaud syndrome.
Women are more likely than men to have Raynaud's disease. It seems to be more common in people who live in colder climates.
Treatment of Raynaud's disease depends on its severity and whether you have other health conditions. For most people, Raynaud's disease isn't disabling, but it can affect your quality of life.
Symptoms
Symptoms of Raynaud's disease include:
- Cold fingers or toes.
- Areas of skin that turn white then blue. Depending on your skin color, these color changes may be harder or easier to see.
- Numb, prickly feeling or stinging pain upon warming or stress relief.
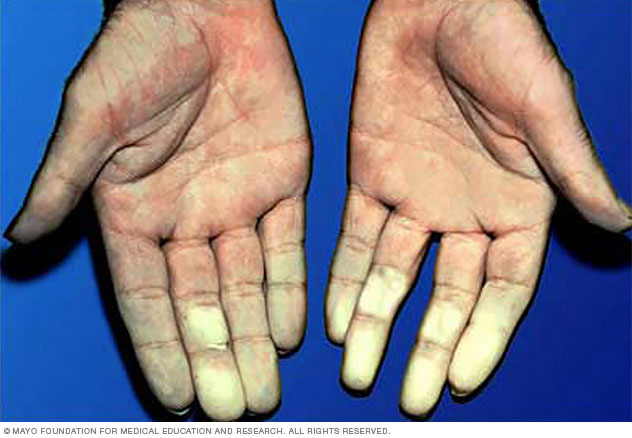
During an attack of Raynaud's, affected areas of the skin usually first turn pale. Next, they often change color and feel cold and numb. When the skin warms and blood flow improves, the affected areas may change color again, throb, tingle or swell.
Raynaud's most commonly affects fingers and toes. But it also can affect other areas of the body, such as nose, lips, ears and even nipples. After warming up, the return of blood flow to the area can take 15 minutes.
When to see a doctor
See your health care provider right away if you have a history of severe Raynaud's and get a sore or infection in one of your affected fingers or toes.
Causes
Experts don't fully understand the cause of Raynaud's attacks. But blood vessels in the hands and feet appear to react too strongly to cold temperatures or stress.
With Raynaud's, arteries to the fingers and toes narrow when exposed to cold or stress. The narrowed arteries limit blood flow. Over time, these small arteries can thicken slightly and limit blood flow even more.
Cold temperatures are the most likely cause of an attack. Examples are putting hands in cold water, taking something from a freezer or being in cold air. For some people, emotional stress can trigger an episode.
Primary vs. secondary Raynaud's
There are two main types of the condition.
- Primary Raynaud's. Also called Raynaud's disease, this most common form isn't the result of another medical condition. It can be so mild that many people with primary Raynaud's don't seek treatment. And it can go away on its own.
-
Secondary Raynaud's. Also called Raynaud's phenomenon, this form develops because of another health condition. Although secondary Raynaud's is less common than the primary form, it tends to be more serious.
Symptoms of secondary Raynaud's usually appear around age 40. That's later than symptoms appear for primary Raynaud's.
Causes of secondary Raynaud's include:
- Connective tissue diseases. Most people who have a rare disease that leads to hardening and scarring of the skin, known as scleroderma, have Raynaud's. Other diseases that increase the risk of Raynaud's include lupus, rheumatoid arthritis and Sjogren's syndrome.
- Diseases of the arteries. These include a buildup of fatty deposits in blood vessels that feed the heart and a disorder in which the blood vessels of the hands and feet become inflamed. A type of high blood pressure that affects the arteries of the lungs also may cause secondary Raynaud's.
- Carpal tunnel syndrome. This condition involves pressure on a major nerve to the hand. The pressure causes numbness and pain in the hand that can make the hand react more to cold temperatures.
- Repeated actions or vibration. Typing, playing piano or doing movements like that for long periods can cause overuse injuries. So can using vibrating tools, such as jackhammers.
- Smoking. Smoking narrows blood vessels.
- Injuries to the hands or feet. Examples include a wrist fracture, surgery or frostbite.
- Certain medicines. These include beta blockers for high blood pressure, some migraine medicines, attention-deficit/hyperactivity disorder medicines, certain cancer medicines and some cold medicines.
Risk factors
Risk factors for primary Raynaud's include:
- Sex. The condition affects more women than men.
- Age. Although anyone can develop the condition, primary Raynaud's often begins between the ages of 15 and 30.
- Climate. The illness also is more common in people who live in colder climates.
- Family history. Having a parent, sibling or child with the disease appears to increase the risk of primary Raynaud's.
Risk factors for secondary Raynaud's include:
- Certain diseases. These include conditions such as scleroderma and lupus.
- Certain jobs. These include jobs that cause repeated trauma, such as using tools that vibrate.
- Certain substances. This includes smoking, taking medicines that affect the blood vessels and being around certain chemicals, such as vinyl chloride.
Complications
If secondary Raynaud's is severe, reduced blood flow to fingers or toes could cause tissue damage. But that's rare.
A completely blocked artery can lead to skin sores or dead tissue. This can be difficult to treat. Rarely, very bad untreated instances might require removing the affected part of the body.
Prevention
To help prevent Raynaud's attacks:
-
Bundle up outdoors. When it's cold, wear a hat, scarf, socks and boots, and two sets of mittens or gloves. Thermal underwear might help. A coat with cuffs that close around mittens or gloves helps protect the hands from cold air.
Wear earmuffs and a face mask if the tip of your nose and your earlobes get too cold.
- Warm your car. Run your car heater for a few minutes before driving in cold weather.
-
Take care indoors. Wear socks. To take food out of the refrigerator or freezer, wear gloves, mittens or oven mitts. Some people find it helpful to wear mittens and socks to bed during winter.
Because air conditioning can cause attacks, set your air conditioner to a warmer temperature. Use drinking glasses that keep hands from feeling cold.
Diagnosis
Your health care provider asks about your symptoms and medical history and does a physical exam. You also might have tests to rule out other medical problems that can cause similar symptoms.
Tests
A test called nailfold capillaroscopy can tell the difference between primary and secondary Raynaud's. During the test, the provider uses a microscope or magnifier to look for anything unusual on the skin at the base of a fingernail. This might include swelling of the blood vessels.
Blood tests can help determine whether another condition, such as an autoimmune condition or a connective tissue disease, is causing Raynaud's. Blood tests for Raynaud's might include:
- Antinuclear antibodies test, also called an ANA test. A positive test result often means that your immune system is mistakenly attacking body tissue. This is called an autoimmune reaction. Such immune system activity is common in people who have connective tissue diseases or other autoimmune disorders.
- Erythrocyte sedimentation rate. This test shows the rate at which red blood cells fall to the bottom of a tube. A faster than typical rate might signal an inflammatory or autoimmune disease.
No one blood test can diagnose Raynaud's. Other tests, such as those that rule out diseases of the arteries, can help find a condition that can be related to Raynaud's.
Treatment
Dressing for the cold in layers and wearing gloves or heavy socks usually can help mild symptoms of Raynaud's. Medicines can treat more-severe symptoms. The goals of Raynaud's treatment are to:
- Reduce the number and severity of attacks.
- Prevent tissue damage.
- Treat the underlying disease or condition.
Medications
Depending on the cause of symptoms, medicines might help. Medicines used to treat people with Raynaud's disease may include:
- Calcium channel blockers. These drugs relax and open small blood vessels in the hands and feet. These drugs also can help heal sores on fingers or toes. Examples include nifedipine (Procardia), amlodipine (Norvasc), felodipine and isradipine.
- Vasodilators. These drugs relax blood vessels. They include the high blood pressure drug losartan (Cozaar), the erectile dysfunction medicine sildenafil (Viagra, Revatio), the antidepressant fluoxetine (Prozac) and a class of medicines called prostaglandins.
Surgeries and medical procedures
Surgery or shots might be needed to treat severe Raynaud's.
-
Nerve surgery. Nerves in the hands and feet control opening and narrowing of blood vessels in skin. Cutting these nerves stops those responses.
Through small incisions in the affected hands or feet, a provider strips tiny nerves around the blood vessels. This surgery, if successful, might lead to fewer and shorter attacks.
- Chemical injection. Shots of numbing medicines or onabotulinumtoxinA (Botox) can block nerves in affected hands or feet. Some people need to have this more than once if symptoms remain or return.
Lifestyle and home remedies
You take steps to decrease Raynaud's attacks and help you feel better.
- Avoid smoke. Smoking, vaping or breathing in someone else's smoke tightens blood vessels. This causes skin temperature to drop.
- Exercise. Exercise increases blood flow. And it's has many other health benefits. If you have secondary Raynaud's, talk to your health care provider before exercising outdoors in the cold.
- Manage stress. Stress can trigger Raynaud's symptoms. Find ways to help reduce emotional stress. Getting more exercise, practicing mindfulness and joining support groups are some ways to reduce and manage stress.
- Avoid rapidly changing temperatures. Try not to go quickly from heat to air conditioning.
What to do during an attack
Warm your hands, feet or other affected areas. Do the following to gently warm your fingers and toes:
- Get indoors or to a warmer area.
- Wiggle your fingers and toes.
- Place hands under armpits.
- Make wide circles with your arms.
- Run warm — not hot — water over your fingers and toes.
- Massage your hands and feet.
If stress triggers an attack, get away from the stress and relax. Practice a stress-relieving technique that works for you. Warm your hands or feet in water to help lessen the attack.
Alternative medicine
Certain practices and supplements that help blood flow better might help manage Raynaud's. However, alternative medicine practices need more study to know how much they can help Raynaud's. If you're interested, talk to your health care provider about:
- Fish oil. Taking fish oil supplements could increase blood flow.
- Ginkgo. Ginkgo supplements could help lessen the number of Raynaud's attacks.
- Acupuncture. This practice seems to improve blood flow, so it may help Raynaud's attacks.
- Biofeedback. Using the mind to control body temperature might help Raynaud's. Biofeedback includes guided imagery to raise the temperature of hands and feet, deep breathing, and other exercises for relaxing. Your health care provider may be able to suggest a therapist who can help you learn biofeedback techniques. There are books and videos on the subject.
Talk to your provider if you're thinking of trying alternative treatments. Your provider can warn you if there are possible side effects.
Preparing for an appointment
Your primary health care provider will likely be able to diagnose Raynaud's based on your symptoms. You may be referred to a provider trained in disorders of the joints, bones and muscles. This type of health care provider is called a rheumatologist.
Here's information to help you get ready for your appointment.
Make a list of:
- Your symptoms, when they began and what seems to trigger them.
- Other medical conditions you and your family have, particularly connective tissue or autoimmune disorders.
- All medicines, vitamins and other supplements you take, including doses.
- Questions to ask your provider.
Take a family member or friend along, if possible, to help you remember the information you receive.
Questions to ask your provider include:
- What is likely causing my symptoms?
- If I have Raynaud's, is it primary or secondary?
- What treatment do you recommend, if any?
- How can I reduce the risk of a Raynaud's attack?
- I have other health conditions. How can I manage them together?
Don't hesitate to ask other questions.
What to expect from your doctor
Your provider is likely to ask you questions, including:
- During a Raynaud's attack, do your fingers or toes change color or feel numb or painful?
- Has anyone else in your family been diagnosed with Raynaud's?
- Do you smoke?
- How much caffeine, if any, do you have daily?
- What do you do for a living and for recreation?
© 1998-2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use


