Overview
Swimmer's itch is a rash that can occur after you go swimming or wading outdoors. It's most common after being in freshwater lakes and ponds, but you can get it in saltwater too.
Swimmer's itch is usually caused by a reaction to tiny parasites in the water that burrow into your skin while you're swimming or wading in warm, calm water. These parasites can't survive in people, so they soon die.
Swimmer's itch usually clears on its own within a few days. In the meantime, you can control itching with medicine.
Symptoms
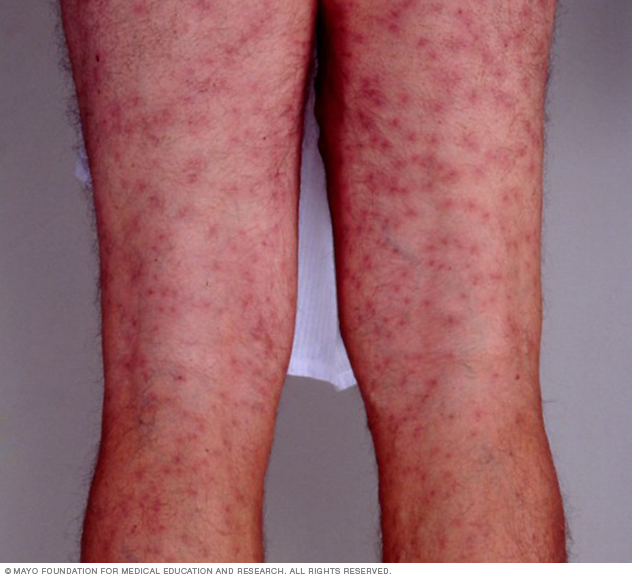
Swimmer's itch symptoms include an itchy rash that looks like pimples or blisters. Symptoms may begin within minutes or as long as two days after swimming or wading in contaminated water.
Usually the rash affects skin that's not covered by swimsuits, wetsuits or waders. Your sensitivity to swimmer's itch can increase each time you're exposed to the parasites that cause it.
When to see a doctor
Talk to your health care provider if you have a rash after swimming that lasts more than a week. If you notice pus at the rash site, check with your health care provider. You might be referred to a doctor who specializes in skin conditions (dermatologist).
Causes
Swimmer's itch is caused by an allergic reaction to parasites that burrow into your skin from warm water. These parasites are found in some animals that live near ponds and lakes, including geese, ducks and muskrats.
The parasites' eggs get into the water through the animals' waste. When the young parasites hatch, they live and grow in a type of snail that lives in shallow water. The snails then release the parasites into the water, where they can infect humans.
Swimmer's itch isn't contagious from person to person.
Risk factors
Factors that can increase the risk of swimmer's itch include:
- Spending time in water that's infested with certain parasites.
- Forgetting to dry off with a towel after getting out of the water.
- Being sensitive to the parasites that cause swimmer's itch.
Complications
Swimmer's itch usually isn't serious, but your skin can become infected if you scratch the rash.
Prevention
Follow these tips to avoid swimmer's itch:
- Choose swimming spots carefully. Avoid being in water near the shore where swimmer's itch is a known problem or where signs have been posted warning of the risk. Also avoid being in marshy areas where snails are often found.
- Rinse after swimming. Rinse exposed skin with clean water right after leaving the water. Then dry the skin with a towel.
- Skip the bread crumbs. Don't feed birds on piers or near swimming areas.
Diagnosis
Your health care provider will likely diagnose swimmer's itch by looking at your skin and talking with you about your activities and symptoms. The condition can look like poison ivy rash and other skin conditions. There are no specific tests to diagnose swimmer's itch.
Treatment
Swimmer's itch typically clears up on its own within a week. If the itching is severe, your health care provider may recommend prescription-strength lotions or creams.
Lifestyle and home remedies
These tips might help reduce the itch:
- Apply a corticosteroid cream or an anti-itch lotion, such as those that contain calamine.
- Take an oral nonprescription antihistamine (Benadryl) or one with loratadine (Alavert, Claritin, others). The latter type causes less sleepiness than does Benadryl.
- Avoiding scratching the rash.
- Cover affected areas with a clean, damp washcloth.
- Soak in a bath sprinkled with Epsom salts, baking soda or an oatmeal-based bath product (Aveeno, others).
- Make a paste of baking soda and water, and then apply it to the affected skin.
Preparing for an appointment
You're likely to start by seeing your primary health care provider. Or you may be referred immediately to a specialist in skin conditions (dermatologist).
What you can do
Before your appointment, you might want to write a list of answers to the following questions:
- When did you first begin experiencing symptoms?
- Have you been swimming or wading outdoors recently?
- Did anyone else who went swimming with you develop a rash?
- What medications and supplements do you take regularly?
What to expect from your doctor
Your health care provider is likely to ask you a number of questions, such as:
- Have your symptoms been continuous or occasional?
- What, if anything, seems to improve your symptoms?
- What, if anything, seems to worsen your symptoms?
© 1998-2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use


