Overview
Trigeminal neuralgia (try-JEM-ih-nul nu-RAL-juh) is a condition that causes intense pain similar to an electric shock on one side of the face. It affects the trigeminal nerve, which carries signals from the face to the brain. Even light touch from brushing your teeth or putting on makeup may trigger a jolt of pain. Trigeminal neuralgia can be long-lasting. It's known as a chronic pain condition.
People with trigeminal neuralgia may at first experience short, mild episodes of pain. But the condition can get worse, causing longer periods of pain that happen more often. It's more common in women and people older than 50.
But trigeminal neuralgia, also known as tic douloureux, doesn't mean living a life of pain. It usually can be managed with treatment.
Symptoms
Trigeminal neuralgia symptoms may include one or more of these patterns:
- Episodes of intense shooting or jabbing pain that may feel like an electric shock.
- Sudden episodes of pain or pain triggered by touching the face, chewing, speaking or brushing your teeth.
- Episodes of pain lasting from a few seconds to several minutes.
- Pain that occurs with facial spasms.
- Episodes of pain lasting days, weeks, months or longer. Some people have periods when they experience no pain.
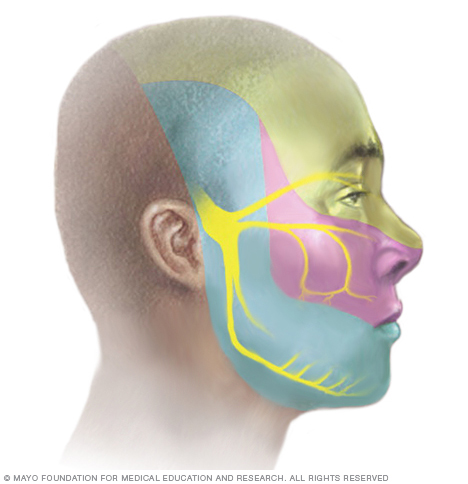
- Pain in areas supplied by the trigeminal nerve. These areas include the cheek, jaw, teeth, gums or lips. Less often, the eye and forehead may be affected.
- Pain on one side of the face at a time.
- Pain focused in one spot. Or the pain may be spread in a wider pattern.
- Pain that rarely occurs while sleeping.
- Episodes of pain that become more frequent and intense over time.
When to see a doctor
See your healthcare professional if you experience pain in your face, particularly if it's long-lasting or comes back after going away. Also get medical attention if you have chronic pain that doesn't go away with pain medicine that you buy off the shelf.
Causes
In trigeminal neuralgia, the trigeminal nerve's function is disrupted. Contact between a blood vessel and the trigeminal nerve at the base of the brain often causes the pain. The blood vessel may be an artery or a vein. This contact puts pressure on the nerve and doesn't allow it to function as usual.
But while compression by a blood vessel is a common cause, there are many other potential causes. Multiple sclerosis or a similar condition that damages the myelin sheath protecting certain nerves can cause trigeminal neuralgia. A tumor pressing against the trigeminal nerve also can cause the condition.
Some people may experience trigeminal neuralgia as a result of a stroke or facial trauma. An injury of the nerve due to surgery also can cause trigeminal neuralgia.
Triggers
Several triggers may set off the pain of trigeminal neuralgia, including:
- Shaving.
- Touching your face.
- Eating.
- Drinking.
- Brushing your teeth.
- Talking.
- Putting on makeup.
- A light breeze blowing over your face.
- Smiling.
- Washing your face.

Diagnosis
Your healthcare professional diagnoses trigeminal neuralgia mainly based on your description of the pain, including:
- Type. Pain related to trigeminal neuralgia is sudden, feels like an electric shock and is brief.
- Location. The parts of your face affected by pain can tell your healthcare professional if the trigeminal nerve is involved.
- Triggers. Eating, talking, light touch of your face or even a cool breeze can bring on pain.
Your healthcare professional may conduct tests to diagnose trigeminal neuralgia. Tests also can help find the causes of the condition. They may include:
- A neurological exam. Touching and examining parts of your face can help determine exactly where the pain is occurring. If you appear to have trigeminal neuralgia, the exam can help uncover which branches of the trigeminal nerve may be affected. Reflex tests can help determine if your symptoms are caused by a compressed nerve or another condition.
- Magnetic resonance imaging (MRI). You may need an MRI to look for possible causes of trigeminal neuralgia. An MRI may reveal signs of multiple sclerosis or a tumor. Sometimes a dye is injected into a blood vessel to view the arteries and veins to show blood flow.
Your facial pain may be caused by many different conditions, so an accurate diagnosis is important. Your healthcare professional also may order other tests to rule out other conditions.
Treatment
Trigeminal neuralgia treatment usually starts with medications, and some people don't need any additional treatment. However, over time, some people with the condition may stop responding to medications, or they may experience unpleasant side effects. For those people, injections or surgery provide other trigeminal neuralgia treatment options.
If your condition is due to another cause, such as multiple sclerosis, you need treatment for the underlying condition.
Medications
To treat trigeminal neuralgia, healthcare professionals prescribe medicines to lessen or block the pain signals sent to your brain.
-
Anti-seizure medicines. Healthcare professionals often prescribe carbamazepine (Tegretol, Carbatrol, others) for trigeminal neuralgia. It has been shown to be effective in treating the condition.
Other anti-seizure medicines that may be used include oxcarbazepine (Trileptal, Oxtellar XR), lamotrigine (Lamictal), and phenytoin (Dilantin, Phenytek, Cerebyx). Other medicines that may be used include topiramate (Qudexy XR, Topamax, others), pregabalin (Lyrica) and gabapentin (Neurontin, Gralise, Horizant).
If the anti-seizure medicine you're using becomes less effective, your healthcare professional may increase the dose or switch to another type. Side effects of anti-seizure medicines may include dizziness, confusion, drowsiness and nausea. Also, carbamazepine can trigger a serious reaction in some people, mainly in those of Asian descent. Genetic testing may be recommended before you start carbamazepine.
- Muscle relaxants. Muscle-relaxing medicines such as baclofen (Gablofen, Fleqsuvy, others) may be used alone or in combination with carbamazepine. Side effects may include confusion, nausea and drowsiness.
- Botox injections. Small studies have shown that onabotulinumtoxinA (Botox) injections may reduce pain from trigeminal neuralgia in people who are no longer helped by medicines. However, more research needs to be done before this treatment is widely used for this condition.
Surgery
Surgical options for trigeminal neuralgia include:
-
Microvascular decompression. This procedure involves moving or removing blood vessels that touch the trigeminal nerve to stop the nerve from malfunctioning. A cut, known as an incision, is made behind the ear on the side where you feel the pain. Then, through a small hole in your skull, your surgeon moves any arteries that are in contact with the trigeminal nerve. The surgeon also places a soft cushion between the nerve and the arteries.
If a vein is compressing the nerve, your surgeon may remove it. Part of the trigeminal nerve may be cut if arteries aren't pressing on the nerve. This is known as a neurectomy.
Microvascular decompression can stop or reduce pain for many years. Long-term pain relief depends on the location of pain, type of pain and age of the person. People with a blood vessel that is seen to be compressing the nerve can remain pain free for years after the procedure. Only a small number of people may have pain come back in 3 to 5 years after surgery. Microvascular decompression has some risks, including decreased hearing, facial weakness, facial numbness, stroke or other complications. Most people who have this procedure have no facial numbness afterward.
-
Brain stereotactic radiosurgery, also known as Gamma Knife. In this procedure, a surgeon aims a focused dose of radiation to the root of the trigeminal nerve. The radiation damages the trigeminal nerve to reduce or stop pain. Pain relief occurs gradually and may take up to a month.
Brain stereotactic radiosurgery is successful in stopping pain for most people. But like all procedures, there is a risk that pain may come back, often within 3 to 5 years. If pain returns, the procedure can be repeated or you may have another procedure. Facial numbness is a common side effect, and may occur months or years after the procedure.
Other procedures may be used to treat trigeminal neuralgia, such as a rhizotomy. In a rhizotomy, your surgeon destroys nerve fibers to reduce pain. This causes some facial numbness. Types of rhizotomy include:
-
Glycerol injection. A needle that goes through the face and into an opening in the base of the skull delivers medicine to reduce pain. The needle is guided to a small sac of spinal fluid that surrounds the area where the trigeminal nerve divides into three branches. Then a small amount of sterile glycerol is injected. The glycerol damages the trigeminal nerve and blocks pain signals.
This procedure often relieves pain. However, pain returns in some people. Many people experience facial numbness or tingling after a glycerol injection.
-
Balloon compression. This procedure involves inserting a hollow needle through the face. It's guided it to a part of the trigeminal nerve that goes through the base of the skull. Then a thin, flexible tube called a catheter with a balloon on the end is threaded through the needle. The balloon inflates with enough pressure to damage the trigeminal nerve and block pain signals.
Balloon compression successfully controls pain in most people, at least for a period of time. Most people undergoing this procedure experience at least some temporary facial numbness.
-
Radiofrequency thermal lesioning. This procedure selectively destroys nerve fibers associated with pain. While you're sedated, your surgeon inserts a hollow needle through your face. The surgeon guides the needle to a part of the trigeminal nerve that goes through an opening at the base of your skull.
Once the needle is positioned, your surgeon briefly wakes you from sedation. Your surgeon inserts an electrode through the needle and sends a mild electrical current through the tip of the electrode. You're asked to say when and where you feel tingling.
When your surgeon locates the part of the nerve involved in your pain, you're returned to sedation. Then the electrode is heated until it damages the nerve fibers, creating an area of injury known as a lesion. If the lesion doesn't get rid of your pain, your doctor may create additional lesions.
Radiofrequency thermal lesioning usually results in some temporary facial numbness after the procedure. Pain may return after 3 to 4 years.
Alternative medicine
Alternative treatments for trigeminal neuralgia haven't been as well studied as medicines or surgical procedures. There's often little evidence to support their use.
However, some people have found improvement with treatments such as acupuncture, biofeedback, chiropractic, and vitamin or nutritional therapy. Be sure to check with your doctor before trying an alternative treatment because it may interact with your other treatments.
Coping and support
Living with trigeminal neuralgia can be difficult. The disorder may affect your interaction with friends and family, your productivity at work, and the overall quality of your life.
You may find encouragement and understanding in a support group. Group members often know about the latest treatments and tend to share their own experiences. If you're interested, your doctor may be able to recommend a group in your area.
Preparing for an appointment
Make an appointment with your healthcare professional if you have symptoms of trigeminal neuralgia. After your initial visit, you may see a doctor trained in brain and nervous system conditions, known as a neurologist.
What you can do to prepare
- Write down any symptoms you've been having, and for how long.
- Note any triggers that bring on facial pain.
- Make a list of your key medical information, including any other conditions for which you're being treated. Also include the names of any medicines, vitamins or supplements you're taking.
- Take a family member or friend along, if possible. Someone who comes with you may remember something that you missed or forgot.
- Write down your questions in advance. It can help you make the most of your time with your healthcare professional.
For possible trigeminal neuralgia, some basic questions to ask include:
- What's the most likely cause of my pain?
- Do I need any diagnostic tests?
- What treatment approach do you recommend?
- If you're recommending medicines, what are the possible side effects?
- Will I need treatment for the rest of my life?
- How much do you expect my symptoms will improve with treatment?
- Is surgery an option?
In addition to the questions that you've prepared, don't hesitate to ask any others that come up during your visit. Also ask questions if you don't understand something.
What to expect from your doctor
You're likely to be asked a number of questions. Being ready to answer them may give you more time to go over points you want to discuss further. Your healthcare professional may ask:
- What are your symptoms and where are they located?
- When did you first develop these symptoms?
- Have your symptoms gotten worse over time?
- How often do you experience periods of facial pain? Have you noticed if anything seems to trigger your facial pain?
- How long does facial pain typically last?
- How much are these symptoms affecting your quality of life?
- Have you ever had dental surgery or surgery on or near your face, such as sinus surgery?
- Have you had any facial trauma, such as an injury or accident that affected your face?
- Have you tried any treatments for your facial pain so far? Has anything helped?
- What side effects have you experienced from treatment?
© 1998-2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use


