Overview
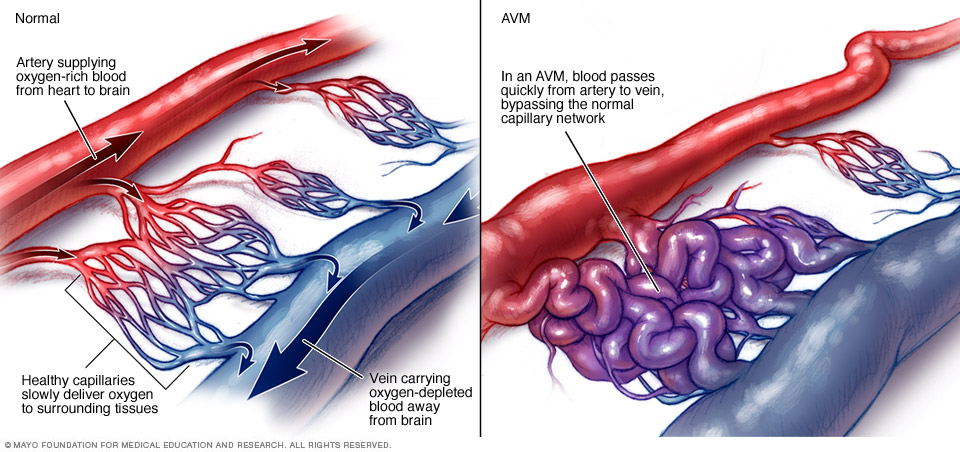
An arteriovenous malformation (AVM) is a tangle of blood vessels that irregularly connects arteries and veins, disrupting blood flow and oxygen circulation. Arteries move oxygen-rich blood from the heart to the brain and other organs. Veins drain the oxygen-depleted blood back to the lungs and heart.
When an AVM disrupts this critical process, the surrounding tissues might not get enough oxygen. Also, because the tangled blood vessels in an AVM do not form properly, they can weaken and rupture. If an AVM in the brain ruptures, it can cause bleeding in the brain, stroke or brain damage. Bleeding in the brain also is called hemorrhage.
Read more about brain AVM (arteriovenous malformation).
The cause of AVMs is not clear. They're rarely hereditary, meaning passed down in families.
Once diagnosed, a brain AVM often can be treated successfully to prevent or reduce the risk of complications.
Symptoms
Symptoms of an AVM vary based on where it's found. Often the first symptoms appear after bleeding occurs. Besides bleeding, symptoms can include:
- Progressive loss of neurological function
- Headaches
- Nausea and vomiting
- Seizures
- Loss of consciousness
Other possible symptoms include:
- Weak muscles
- Paralysis in one part of the body
- Loss of coordination that can cause problems with gait
- Problems performing tasks that require planning
- Weakness in the lower extremities
- Back pain
- Dizziness
- Vision problems, including losing part of the field of vision, loss of control of eye movements or swelling of part of the optic nerve
- Problems with speech or understanding language
- Unusual sensations including numbness, tingling or sudden pain
- Memory loss or dementia
- Hallucinations
- Confusion
Children and teens might have trouble with learning or behavior.
One type of AVM called a vein of Galen defect causes symptoms that appear at or shortly after birth. A vein of Galen defect is situated deep inside the brain. Signs can include:
- A buildup of fluid in the brain that causes enlargement of the head
- Swollen veins on the scalp
- Seizures
- Failure to thrive
- Congestive heart failure
When to see a doctor
Seek medical attention if you have any of the symptoms of an AVM, such as headaches, dizziness, vision problems, seizures, and changes in thinking or neurological function. Many AVMs are found during testing for a different condition, often after a CT scan or an MRI is obtained for reasons not directly related to the AVM.
Causes
AVMs result from the development of irregular connections between arteries and veins, but experts don't understand why this happens. Certain genetic changes might play a role, but most types are not usually inherited, which means passed down in families.
Risk factors
Rarely, having a family history of AVMs can increase your risk. But most types of AVMs aren't inherited.
Certain hereditary conditions can increase your risk of AVM. These include hereditary hemorrhagic telangiectasia, which is also called Osler-Weber-Rendu syndrome.
Complications
The most common complications of an AVM are bleeding and seizures. If left untreated, the bleeding can cause significant neurological damage and may be fatal.
Diagnosis
To diagnose an AVM, your health care provider will review your symptoms and perform a physical examination.
The provider may listen for a sound called bruit. Bruit is a whooshing sound caused by very rapid blood flow through the arteries and veins of an AVM. It sounds like water rushing through a narrow pipe. Bruit can interfere with your hearing or sleep or cause emotional distress.
Tests commonly used to help diagnose AVM include:
- Cerebral angiography. Also called arteriography, this test uses a special dye called a contrast agent injected into an artery. The dye highlights the structure of blood vessels to better show them on X-rays.
- CT scan. These scans use X-rays to create images of the head, brain or spinal cord and can help show bleeding.
- CT angiography (CTA). CTA combines a CT scan with an injection of a special dye to help locate an AVM that is bleeding.
- MRI. An MRI uses powerful magnets and radio waves to show detailed images of the tissues. An MRI can pick up on small changes in these tissues.
- Magnetic resonance angiography (MRA). MRA captures the pattern and the speed and distance of blood flow through the irregular vessels.
Treatment
Treatment for AVM depends on where it is found, the symptoms and the risk of treatment. Sometimes an AVM is monitored with regular imaging tests to watch for changes or problems. Other AVMs require treatment. Determining whether an AVM needs treatment involves factors including whether the AVM:
- Has bled
- Is causing symptoms other than bleeding
- Is in a part of the brain that can safely receive treatment
Medications
Medications can help manage symptoms such as seizures, headaches and back pain.
Surgery
The main treatment for AVM is surgery. Surgery might be recommended if there is a high risk of bleeding. The surgery might completely remove the AVM. This treatment is usually used when the AVM is in an area where surgeons can remove the AVM with little risk of causing significant damage to the brain tissues.
Endovascular embolization is a type of surgery in which the surgeon threads a catheter through the arteries to the AVM. Then a substance is injected to close parts of the AVM to reduce the blood flow. This might also be done before brain surgery or radiosurgery to help reduce the risk of complications.
Sometimes stereotactic radiosurgery is used to treat AVMs. This uses intense, highly focused beams of radiation to damage the blood vessels and stop the blood supply to the AVM.
You and your health care team will discuss whether to treat your AVM, weighing the possible benefits against the risks.
Follow-up
After treatment for an AVM, you might need regular follow-up visits with your health care provider. You might need more imaging tests to make sure that the AVM has been successfully treated and that the malformation has not come back. You'll also need regular imaging tests and follow-up visits with your health care provider if your AVM is being monitored.
Coping and support
Learning that you have an AVM can be frightening. It can make you feel like you have little control over your health. But you can take steps to cope with the emotions that go with your diagnosis and recovery. Consider:
- Learning enough about AVM to make informed decisions about your care. Ask about the size and location of the AVM, and what that means for your treatment options.
- Accept your emotions. Complications of AVM, such as hemorrhage and stroke, can cause emotional problems as well as physical ones. Coming to terms with the diagnosis might help.
- Keep friends and family close. Friends and family can provide the practical support you'll need, such as going with you to care provider appointments, and serve as emotional support.
- Find someone to talk with. Talking to a friend or family member, a counselor, a medical social worker, a clergy member, or a support group about your hopes and fears can be helpful. Ask your health care provider about support groups in your area. Or check your phone book, library or a national organization, such as the American Stroke Association or The Aneurysm and AVM Foundation.
Preparing for an appointment
An AVM might be diagnosed in an emergency situation, immediately after bleeding, also called hemorrhage, or a seizure has occurred. It also can be detected after other symptoms prompt imaging scans.
But in some cases, an AVM is found during diagnosis or treatment of an unrelated medical condition. You might then be referred to a doctor trained in brain and nervous system conditions. This type of doctor is called a neurologist, interventional neuroradiologist or neurosurgeon.
Here are some tips to help you get ready for your appointment.
What you can do
- Be aware of pre-appointment restrictions. When you make the appointment, ask if there's anything you need to do in advance.
- Write down your symptoms, including any that may seem unrelated to the reason for which you scheduled the appointment.
- Make a list of all medications, vitamins and supplements you're taking, including dosages.
- Ask a family member or friend to come with you, if possible. Someone who accompanies you might help you remember the information you're given.
- Write down questions to ask. Don't be afraid to ask questions that may come up during your appointment.
For AVM, some basic questions to ask your health care provider include:
- What are other possible causes for my symptoms?
- What tests are needed to confirm the diagnosis?
- What are my treatment options and the pros and cons for each?
- What results can I expect?
- What kind of follow-up should I expect?
What to expect from your doctor
Your neurologist is likely to ask about your symptoms, if any, conduct a physical examination and schedule tests to confirm the diagnosis.
The tests gather information about the size and location of the AVM to help direct your treatment options. He or she may ask:
- When did your symptoms begin?
- Have your symptoms been continuous or occasional?
- How severe are your symptoms?
- What, if anything, seems to improve your symptoms?
- What, if anything, appears to worsen your symptoms?
© 1998-2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use


