Overview
Peripheral artery disease (also called peripheral arterial disease) is a common condition in which narrowed arteries reduce blood flow to the arms or legs.
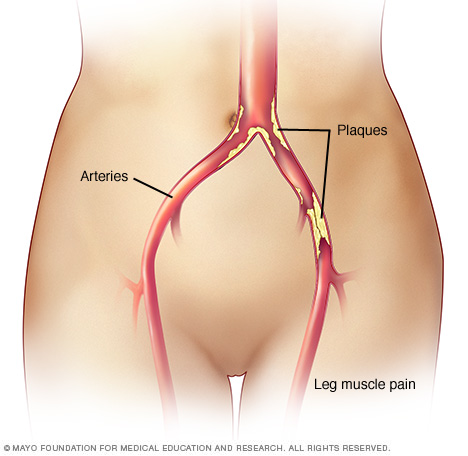
In peripheral artery disease (PAD), the legs or arms — usually the legs — don't receive enough blood flow to keep up with demand. This may cause leg pain when walking (claudication) and other symptoms.
Peripheral artery disease is usually a sign of a buildup of fatty deposits in the arteries (atherosclerosis). Atherosclerosis causes narrowing of the arteries that can reduce blood flow in the legs and, sometimes, the arms.
Peripheral artery disease treatment includes exercising, eating a healthy diet and not smoking or using tobacco.
Symptoms
Many people with peripheral artery disease have mild or no symptoms. Some people have leg pain when walking (claudication).
Claudication symptoms include muscle pain or cramping in the legs or arms that begins during exercise and ends with rest. The pain is most commonly felt in the calf. The pain ranges from mild to severe. Severe leg pain may make it hard to walk or do other types of physical activity.
Other peripheral artery disease symptoms may include:
- Coldness in the lower leg or foot, especially when compared with the other side
- Leg numbness or weakness
- No pulse or a weak pulse in the legs or feet
- Painful cramping in one or both of the hips, thighs or calf muscles after certain activities, such as walking or climbing stairs
- Shiny skin on the legs
- Skin color changes on the legs
- Slower growth of the toenails
- Sores on the toes, feet or legs that won't heal
- Pain when using the arms, such as aching and cramping when knitting, writing or doing other manual tasks
- Erectile dysfunction
- Hair loss or slower hair growth on the legs
If peripheral artery disease gets worse, pain may occur during rest or when lying down. The pain may interrupt sleep. Hanging the legs over the edge of the bed or walking may temporarily relieve the pain.
When to see a doctor
Call your health care provider if you have leg pain, numbness or other symptoms of peripheral artery disease.
Causes
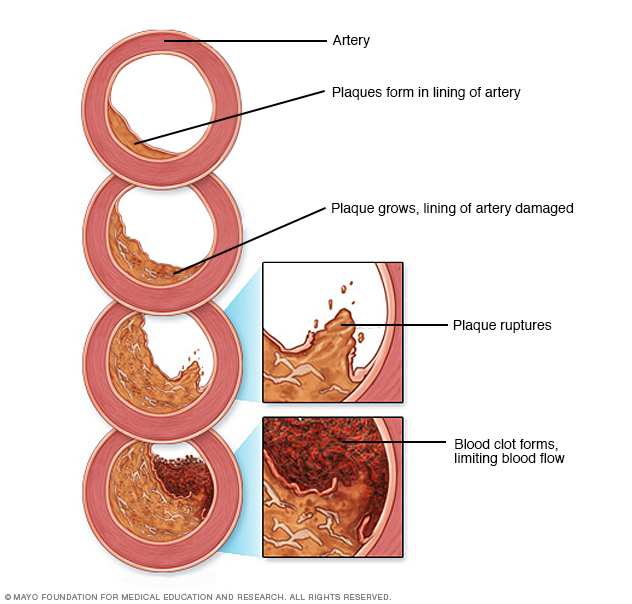
Peripheral artery disease is often caused by a buildup of fatty, cholesterol-containing deposits (plaques) on artery walls. This process is called atherosclerosis. It reduces blood flow through the arteries.
Atherosclerosis affects arteries throughout the body. When it occurs in the arteries supplying blood to the limbs, it causes peripheral artery disease.
Less common causes of peripheral artery disease include:
- Blood vessel inflammation
- Injury to the arms or legs
- Changes in the muscles or ligaments
- Radiation exposure
Risk factors
Smoking or having diabetes greatly increases the risk of developing peripheral artery disease.Other things that increase the risk of peripheral artery disease include:
- A family history of peripheral artery disease, heart disease or stroke
- High blood pressure
- High cholesterol
- High levels of an amino acid called homocysteine, which increase the risk for coronary artery disease
- Increasing age, especially after 65 (or after 50 if you have risk factors for atherosclerosis)
- Obesity (a body mass index over 30)
Complications
Complications of peripheral artery disease caused by atherosclerosis include:
- Critical limb ischemia. In this condition, an injury or infection causes tissue to die. Symptoms include open sores on the limbs that don't heal. Treatment may include amputation of the affected limb.
- Stroke and heart attack. Plaque buildup in the arteries can also affect the blood vessels in the heart and brain.
Prevention
The best way to prevent leg pain due to peripheral artery disease is to maintain a healthy lifestyle. That means:
- Don't smoke.
- Control blood sugar.
- Eat foods that are low in saturated fat.
- Get regular exercise — but check with your care provider about what type and how much is best for you.
- Maintain a healthy weight.
- Manage blood pressure and cholesterol.
Diagnosis
To diagnose peripheral artery disease, a health care provider will examine you. You'll usually be asked questions about your symptoms and medical history.
If you have peripheral artery disease, the pulse in the affected area may be weak or missing.
Tests
Tests that may be done to diagnose peripheral artery disease include:
- Blood tests. Blood tests are done to check for conditions related to PAD such as high cholesterol, high triglycerides and diabetes.
- Ankle-brachial index (ABI). This is a common test used to diagnose PAD. It compares the blood pressure in the ankle with the blood pressure in the arm. You may be asked to walk on a treadmill. Blood pressure readings may be taken before and immediately after exercising to check the arteries during walking.
- Ultrasound of the legs or feet. This test uses sound waves to see how blood moves through the blood vessels. Doppler ultrasound is a special type of ultrasound used to spot blocked or narrowed arteries.
- Angiography. This test uses X-rays, magnetic resonance imaging (MRI) scans or computerized tomography (CT) scans to look for blockages in the arteries. Before the images are taken, dye (contrast) is injected into a blood vessel. The dye helps the arteries show up more clearly on the test images.
Treatment
The goals of treatment for peripheral artery disease are:
- Manage symptoms, such as leg pain, so exercise isn't uncomfortable
- Improve artery health to reduce the risk of heart attack and stroke
Treatments for peripheral artery disease includes lifestyle changes and sometimes, medication.
Lifestyle changes can help improve symptoms, especially early in the course of peripheral artery disease. If you smoke, quitting is the single most important thing you can do to reduce the risk of complications. Walking or doing other exercise on a regular, scheduled basis (supervised exercise training) can improve symptoms dramatically.
Medications
If peripheral artery disease (PAD) is causing symptoms, your provider may prescribe medicine. Medications for PAD may include:
- Cholesterol drugs. Medications called statins are commonly prescribed for people with peripheral artery disease. Statins help lower bad cholesterol and reduce plaque buildup in the arteries. The drugs also lower the risk of heart attacks and strokes. If you have PAD, ask your provider what your cholesterol numbers should be.
- Blood pressure drugs. Uncontrolled high blood pressure can make arteries stiff and hard. This can slow the flow of blood. Ask your health care provider what blood pressure goal is best for you. If you have high blood pressure, your provider may prescribe medications to lower it.
- Medications to control blood sugar. If you have diabetes, controlling your blood sugar levels becomes even more important. Talk with your provider about your blood sugar goals and how to reach them.
- Medications to prevent blood clots. Peripheral artery disease is related to reduced blood flow to the limbs. So, medicines may be given to improve blood flow. Aspirin or another medication, such as clopidogrel (Plavix), may be used to prevent blood clotting.
- Medications for leg pain. The drug cilostazol thins the blood and widens blood vessels. It increases blood flow to the limbs. The drug specifically helps treat leg pain in people who have peripheral artery disease. Common side effects of this medication include headache and diarrhea. An alternative medication is pentoxifylline. Side effects are rare with this medication, but it generally doesn't work as well as cilostazol.
Surgeries or other procedures
In some cases, angioplasty or surgery may be necessary to treat peripheral artery disease that's causing claudication:
- Angioplasty and stent placement. This procedure is done to open clogged arteries. It can diagnose and treat a blocked vessel at the same time. The health care provider guides a thin, flexible tube (catheter) to the narrowed part of the artery. A tiny balloon is inflated to widen the blocked artery and improve blood flow. A small wire mesh tube (stent) may be placed in the artery to keep the artery open.
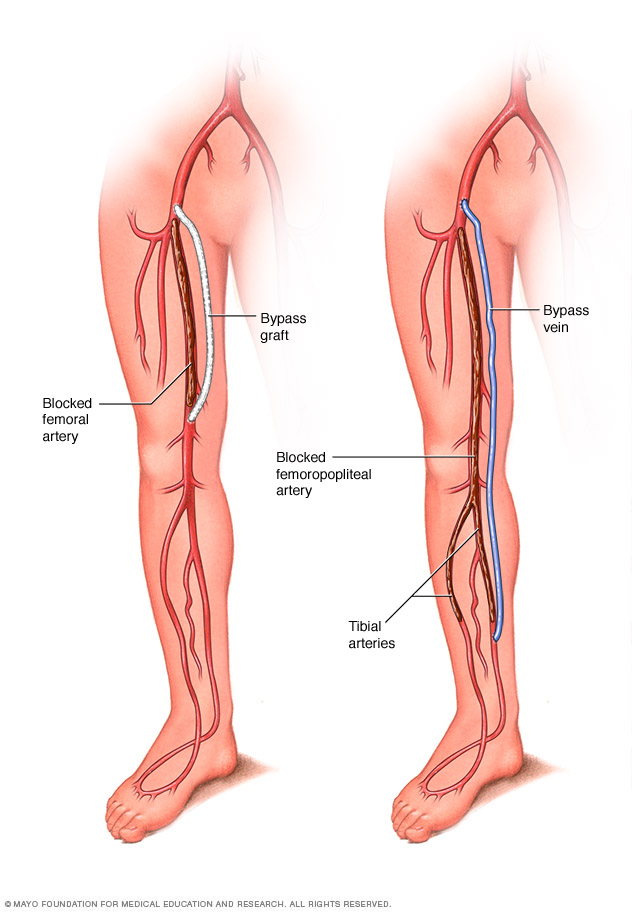
- Bypass surgery. The surgeon creates a path around the blocked artery using either a healthy blood vessel from another part of the body or a synthetic one.
- Thrombolytic therapy. If a blood clot is blocking an artery, a clot-dissolving drug may be given directly into the affected artery.
Lifestyle and home remedies
Making healthy lifestyle changes can help you manage peripheral artery disease symptoms and prevent them from getting worse. Try these tips:
- Don't smoke. Smoking damages the arteries. It increases the risk for peripheral artery disease (PAD). If you have PAD, smoking can make the condition worse. If you need help quitting smoking, ask your care provider about strategies and medications that can help.
- Eat a healthy diet. A heart-healthy diet low in saturated fat helps control blood pressure and cholesterol levels.
- Avoid certain cold and sinus medications. Products that contain pseudoephedrine (Advil Cold and Sinus, Sudafed, others) tighten blood vessels and may increase PAD symptoms.
Exercise
Exercise is an important part of PAD treatment. Regular exercise helps the body use oxygen better and improves symptoms of PAD. Sometimes, the exercise that will help you get better may cause pain. But don't get discouraged. As you continue exercising, you'll be able to walk longer without pain. Your health care provider likely will prescribe supervised exercise therapy to increase the distance you can walk pain-free.
Careful foot care
In addition to lifestyle changes, take good care of your feet. People with PAD, especially those who also have diabetes, are at risk of poor healing of sores and injuries on the lower legs and feet.
Poor blood flow can delay or prevent proper healing. It also increases the risk of infection. Follow this advice to care for your feet:
- Wash your feet every day. Dry them completely. Use moisturizer to prevent cracks that can lead to infection. Don't moisturize between the toes, however, as this can help fungus grow.
- Wear well-fitting shoes and thick, dry socks.
- Promptly treat any fungal infections of the feet, such as athlete's foot.
- Take care when trimming your nails.
- Inspect your feet daily for injuries.
- Have a foot doctor (podiatrist) treat bunions, corns or calluses.
- See your care provider as soon as you notice a sore or injury to your skin.
Also, try sleeping with the head of the bed raised a few inches. Keeping the legs below the level of the heart usually reduces pain.
Preparing for an appointment
You might first visit your family care provider. You may be referred to a doctor who specializes in disorders of blood vessels (vascular specialist) or a doctor trained in heart diseases (cardiologist).
Because appointments can be brief and there's often a lot to discuss, it's a good idea to arrive well prepared. Here's some information to help you get ready for your appointment and know what to expect from your provider.
What you can do
- Write down any symptoms you're having, including any that may seem unrelated to the reason for which you scheduled the appointment.
- Make a list of all medications, vitamins or supplements that you're taking. Include dosages.
- Write down questions to ask your health care provider.
For peripheral artery disease, some basic questions to ask your health care provider include:
- What's the most likely cause of my symptoms?
- Are there other possible causes for my symptoms?
- What kinds of tests do I need? Do these tests require any special preparation?
- Is peripheral artery disease temporary or long lasting?
- What treatments are available, and which do you recommend?
- What types of side effects can I expect from treatment?
- Are there any alternatives to the primary approach that you're suggesting?
- What can I do on my own that might help me get better?
- I have other health conditions. How can I best manage these conditions together?
- Is there a generic alternative to the medicine you're prescribing me?
- Are there any brochures or other printed material that I can take home with me? What websites do you recommend visiting?
Don't hesitate to ask additional questions during your appointment if you don't understand something.
What to expect from your doctor
Your health care provider is likely to ask you many questions. Being ready to answer them may save time to go over any details you want to spend more time on. Your provider may ask:
- When did the symptoms start?
- Do you always have symptoms or do they come and go?
- How severe are your symptoms?
- Do your symptoms get worse when you exercise?
- Do your symptoms get better when you're resting?
- Do you use tobacco products? If yes, how often?
What you can do in the meantime
If you smoke, quit. Smoking increases the risk of peripheral artery disease and can make existing PAD worse. If you need help quitting, ask your care provider for strategies that can help.
Eating less saturated fat and adding more fruits and vegetables to your diet are two other healthy lifestyle habits you can immediately try.
© 1998-2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use


