Overview
Urinary incontinence is the loss of bladder control. Stress incontinence happens when movement or activity puts pressure on the bladder, causing urine to leak. Movements include coughing, laughing, sneezing, running or heavy lifting. Stress incontinence is not related to mental stress.
Stress incontinence is not the same as urgency incontinence and overactive bladder (OAB). Those conditions cause the bladder muscle to spasm. This leads to a sudden need to urinate quickly. Stress incontinence is much more common in women than in men.
If you have stress incontinence, you may feel ashamed. You might limit your work and social life because you don't want to be with others. You also might not do physical or fun activities.
Treatment can help you manage stress incontinence and improve your quality of life.
Symptoms
If you have stress incontinence, you may leak urine when you:
- Cough or sneeze.
- Laugh.
- Bend over.
- Lift something heavy.
- Exercise.
- Have sex.
You might not leak urine every time you do one of these things. But any activity that puts pressure on your bladder can make leaking more likely. Having a full bladder increases the chances of leaking.
When to see a doctor
Talk to your healthcare professional if your symptoms bother you or get in the way of daily activities like work, hobbies and social life.
Causes
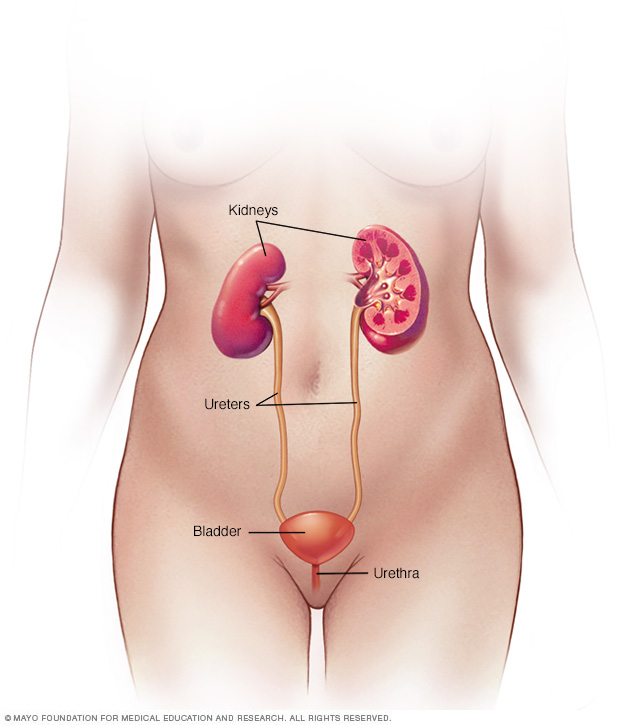
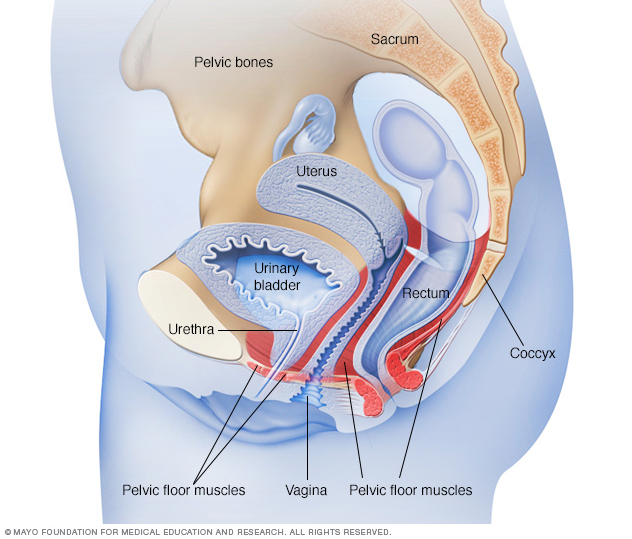
Stress incontinence happens when certain muscles and other tissues linked to urinating weaken. These include the muscles that support the urethra, called the pelvic floor muscles, and the muscles that control the release of urine, called the urinary sphincter.
The bladder expands as it fills with urine. Most often, valve-like muscles in the tube that carries urine out of the body, called the urethra, stay closed as the bladder expands. This keeps you from leaking urine until you reach a bathroom.
But when those muscles weaken, anything that puts force on the stomach and pelvic muscles put pressure on your bladder. Sneezing, bending over, lifting or laughing hard, for instance, can cause urine leakage.
Female stress incontinence
In people assigned female at birth, the pelvic floor muscles and urinary sphincter may lose strength because of:
- Childbirth. Tissue or nerve damage during delivery of a child can weaken the pelvic floor muscles or the sphincter. Stress incontinence from this damage may begin soon after delivery or happen years later.
Male stress incontinence
In people assigned male at birth, the pelvic floor muscles and urinary sphincter may lose strength because of:
- Prostate surgery. Treatment for prostate cancer often involves surgery to remove the prostate gland, called a prostatectomy. This surgery is the most common factor leading to stress incontinence. This procedure can weaken the sphincter, which lies right below the prostate gland and goes around the urethra.
Other factors
Other factors that can make stress incontinence worse for males and females include:
- Illnesses that cause chronic coughing.
- Obesity.
Risk factors
Factors that increase the risk of getting stress incontinence include:
- Age. Physical changes that happen with age, such as muscles getting weaker, may make you more likely to get stress incontinence. But some stress incontinence can happen at any age.
- Body weight. People who are overweight or obese have a higher risk of stress incontinence. Excess weight increases pressure on the abdominal and pelvic organs.
For females, risks factors also include:
- Type of childbirth delivery. People who've had a vaginal delivery are more likely to have urinary incontinence than are those who had a cesarean section. Having more than one child also raises the risk.
Complications
Complications of stress incontinence may include:
- Emotional upset. If you have stress incontinence, you may feel embarrassed. It can disrupt your work, social life, relationships and even your sex life. Some people are ashamed that they need pads or incontinence garments.
- Mixed urinary incontinence. It's common to have both stress incontinence and urgency incontinence. Urinary incontinence results when bladder muscles tighten and cause an urgent need to urinate. People with this condition may have frequent urination, urination in the evening and urgency to urinate with or without associated incontinence. This is called overactive bladder.
- Skin rash or soreness. Prolonged contact with urine can cause skin to be sore or to break down. This can happen with severe incontinence if you don't use moisture barriers or incontinence pads. Change pads often and use continence pads rather than menstrual pads to prevent skin sores.
Diagnosis
During your visit, your healthcare professional looks for clues to the cause of your symptoms. Your appointment will likely include:
- Voiding diary that tells how much you drink and when and how often you urinate.
- Medical history.
- Physical exam. This might include a pelvic exam in women and a rectal exam.
- Test of a urine sample for infection or traces of blood.
- Brief neurological exam to see how the pelvic nerves work.
- Urinary stress test, in which your healthcare professional looks for urine loss when you cough or bear down with a full bladder.
Tests of bladder function
Common cases of urinary incontinence often don't need other tests. But sometimes your healthcare professional might order tests to see how well your bladder, urethra and sphincter work.
Bladder function tests may include:
-
Measuring how much urine stays in your bladder after you urinate. You might have this test if there's concern about your being able to empty your bladder all the way. People who are older, have had bladder surgery or have diabetes might need this test.
A specialist uses an ultrasound scan, which turns sound waves into an image. The test shows how much urine is left in your bladder after you urinate. Sometimes, the test involves passing a thin tube called a catheter through your urethra into your bladder. The catheter drains the urine that's left so it can be measured.
-
Measuring bladder pressures. Urodynamics is a test that measures pressure in your bladder during filling and emptying. This test can check for stress incontinence and the strength of the pelvic floor muscles. Some healthcare professionals use these results to choose a surgical approach.
A catheter is used to fill your bladder slowly with warm fluid. As your bladder fills, you may be asked to cough or bear down to test for leaks. This procedure may be used with a pressure-flow study. This shows how much pressure your bladder uses to empty all the way.
- Cystoscopy. This test uses a scope that is put into the bladder to look for conditions in the bladder and urethra that may be causing your symptoms. This procedure is usually done in a medical office.
Treatment
Your healthcare professional may suggest a mix of ways to treat stress incontinence. If you have a urinary tract infection, you get treatment for the condition before starting treatment for stress incontinence.
Behavior therapies
Behavior therapies may help you have less or no stress incontinence. Treatments might include:
-
Pelvic floor muscle exercises. A member of your healthcare team or a physical therapist can help you learn how to do Kegel exercises to strengthen your pelvic floor muscles and urinary sphincter. For Kegel exercises to work, you must do them regularly.
A technique called biofeedback can be used along with Kegel exercises to make exercises work better. Biofeedback involves the use of pressure sensors or electrical stimulation to guide proper muscle contractions. Once your muscles are strong you can squeeze these muscles before doing anything that causes leakage to help keep from leaking.
- Drinking fluids. Your health professional may suggest how much and what type of fluid you should drink during the day and evening and when. But don't limit what you drink so much that your body loses too much fluid, called dehydration.
- Healthy lifestyle changes. Quitting smoking, losing excess weight or treating an ongoing cough will lessen your risk of stress incontinence and improve your symptoms.
- Bladder training. Your health professional might suggest a schedule for using the toilet if you have mixed incontinence. Urinating more often may help with urge incontinence.
Medicines
There's no medicine approved to treat stress incontinence in the United States.
Lifestyle and home remedies
Healthy lifestyle practices can ease symptoms of stress incontinence. These include:
- Shed extra weight. If your body mass index (BMI) is 30 or higher, losing weight can help reduce the pressure on your bladder and pelvic floor muscles. Even a 10% weight loss may greatly improve stress incontinence. Talk to a member of your care team for help with weight loss.
- Add fiber to your diet. Having trouble moving your bowls can add to urinary incontinence. Keeping bowel movements soft and regular eases the strain on your pelvic floor muscles. Try eating high-fiber foods to relieve and prevent constipation. High-fiber foods include whole grains, legumes, fruits and vegetables.
Coping and support
Treatments for stress incontinence often can greatly reduce, and possibly stop, urine leakage. Some people will still have urine leakage every now and then. Being prepared may help you cope.
Going out and about
Stay connected to family, friends and co-workers so you don't feel lonely and sad. Being prepared may help you feel better about being out and about:
-
Stock up on supplies. Take enough incontinence pads or protective undergarments and possibly a change of clothes with you. Incontinence products are small. They can go into a roomy purse or a small backpack.
You can keep extra supplies and spare clothes in the trunk of your car or in a backpack for use when needed.
- Know where you're going. Know where the restrooms are. Choose seating that lets you get to the restrooms easily.
- Take good care of your skin. Long contact with wet clothing can cause skin sores. Keep your skin dry by changing out of wet clothes. Use a barrier cream if your skin is often wet.
Sex and incontinence
Leaking urine during sexual intercourse can be upsetting. But there are ways to keep it from ruining sex for you.
- Talk with your partner. This might be hard to do but tell your partner about your symptoms. A partner's support and being willing to help can make your symptoms easier to handle.
- Empty your bladder before sex. To reduce your chances of leakage, don't drink fluids for an hour or so before sex. Empty your bladder before you start having sex.
- Try another position. Changing positions may make leakage less likely for you. For women, being on top might give better control of the pelvic muscles.
- Do your Kegel exercises. These exercises strengthen your pelvic floor muscles and reduce urine leakage.
- Be prepared. Having towels handy or using disposable pads on your bed may ease your worry and hold leakage.
Seek help
Incontinence is not a usual part of aging. Treatments can cure stress incontinence or greatly reduce its effects on your life.
Find a healthcare professional who will work with you to find the best way to treat your incontinence. You should work together to find the right treatments for you. Take time to talk about the pros and cons of the many treatment options.
You might want to join a support group. Support groups give you a place to talk about your concerns. And they can help keep you going with your self-care efforts.
Groups such as the National Association for Continence offer resources and information for people who have stress incontinence.
Preparing for an appointment
Your healthcare professional may have you fill out a form about your stress incontinence symptoms. You also might be asked to keep a bladder diary for a few days.
In a bladder diary, you write down when, how much and what kind of fluids you consume. You also note how much you urinate and when you have incontinence.
Your diary may show patterns that help your healthcare professional know about your condition. This may reduce the need for some testing.
If you need special tests, you might be sent to a specialist in urinary conditions, called a urologist, or a specialist in women's urinary conditions, called a urogynecologist.
What you can do
To make the most of your appointment, take a family member or friend with you to help you remember the information you get.
Make a list of:
- Your symptoms. Include when urine leakage occurs.
- Any medicines, vitamins or supplements you take. Include doses and how often you take the medicine.
- Questions to ask your healthcare professional.
For urinary incontinence, some questions to ask include:
- Will my urinary incontinence get worse?
- Could pelvic floor exercises help me? How do I do them?
- How does my weight affect my condition?
- Could the medicines I take be making my condition worse?
- What tests might I need to find the cause of my incontinence?
- Will I need surgery?
Be sure to ask all the questions you have.
What to expect from your healthcare professional
Be prepared to answer questions from your healthcare professional, such as:
- How often do you leak urine?
- When you leak urine, is it a few drops or are your clothes soaked?
- Are there times when you know that you will leak?
- Do you leak urine when you exercise?
- Do you wake up during the night to urinate? How often?
- How much do you drink every day?
- Does anything seem to make your incontinence better? How about worse?
- What bothers you most about your urinary incontinence?
- Do you also have bowel leakage? How often? Does this cause you to restrict your activities?
- Does it feel as if something is falling out of your pelvis or vagina?
© 1998-2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use


